INTRODUCTION
Soft tissue augmentation using hyaluronic acid (HA) fillers is widely used to decrease facial lines and improve the appearance of soft tissues. However, varying degrees of complications can occur after HA filler injection [1,2]. Tissue necrosis due to interruption of the vascular supply is an early complication that can be severe [3].
In the present study, we describe a patient with widespread skin necrosis after HA filler injection in the glabellar area. Additionally, we describe a unique flap design inspired by the double-opposing rotation-advancement flap method used by Ransom and Jacono [4]. Using modified double-opposing rotation-advancement flaps, it is possible to achieve adequate soft tissue coverage and minimal free margin distortion when reconstructing widespread skin necrosis in the central mid-lower forehead that can occur after filler injection in the glabellar area.
CASE REPORT
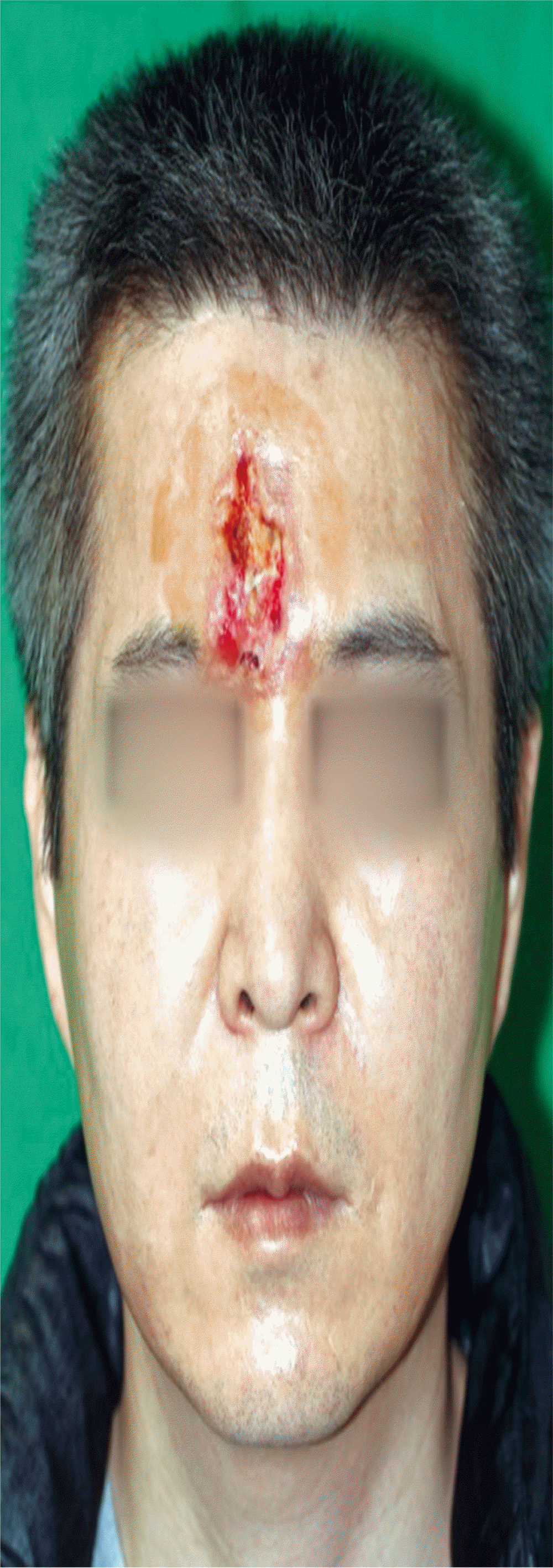
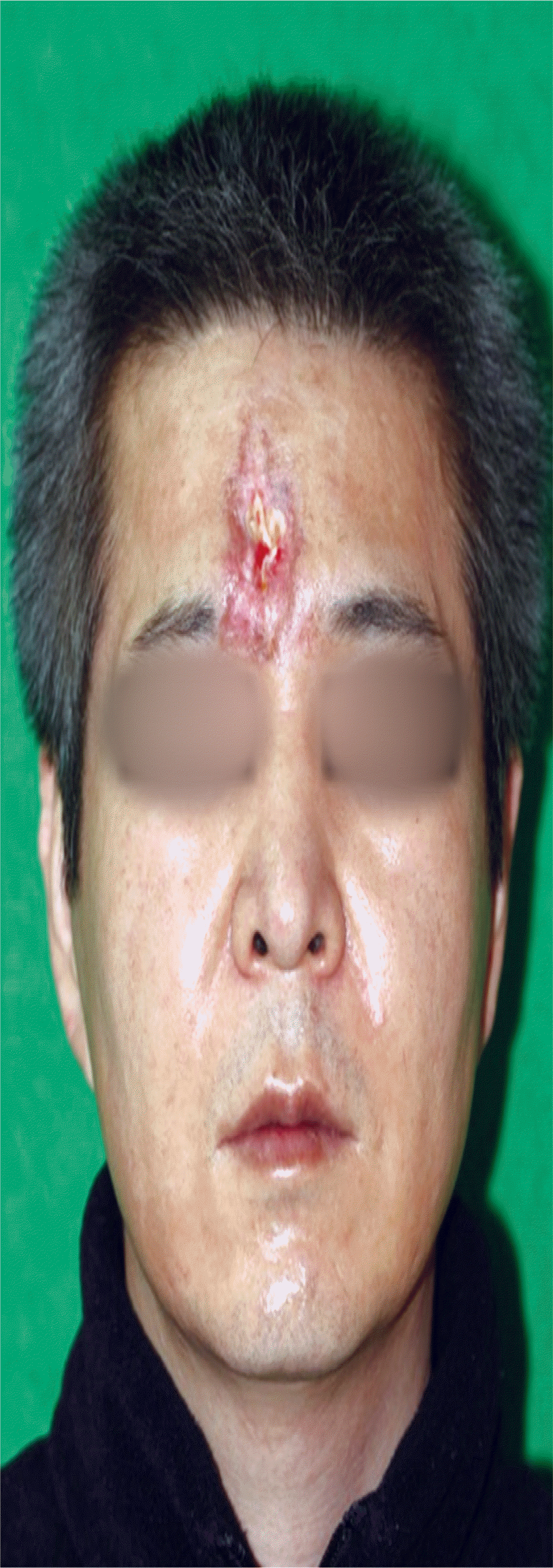
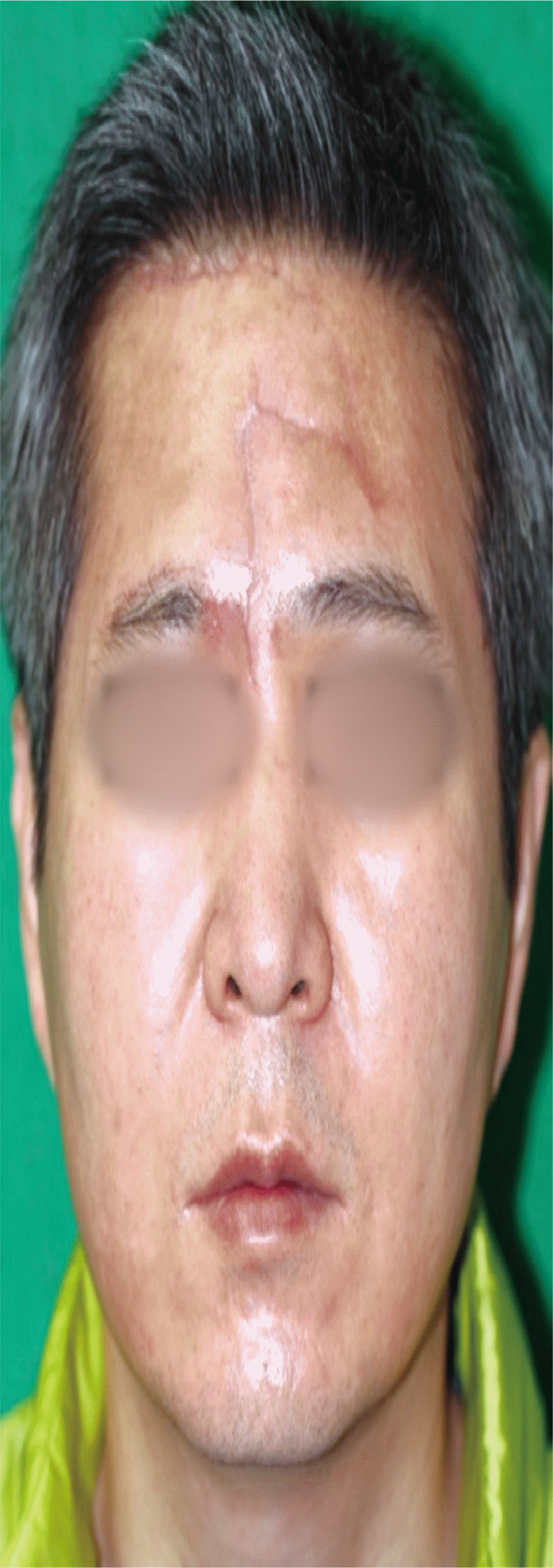
A 50-year-old man presented as an outpatient to the Plastic Surgery Department of Busan Paik Hospital. His main symptom was worsening of skin necrosis immediately after a filler injection that was administered 3 weeks prior at a local clinic to treat frown lines in the glabellar area. Tissue necrosis progressed despite the initial treatment including massage, warm compression, and hyaluronidase injection (Fig. 1). The patient was treated as an outpatient for 2 weeks to confirm the necrosis margin and to facilitate wound healing. Wound healing progressed, but secondary healing produced unacceptable scars. Therefore, he was admitted to the hospital for reconstructive surgery (Fig. 2).
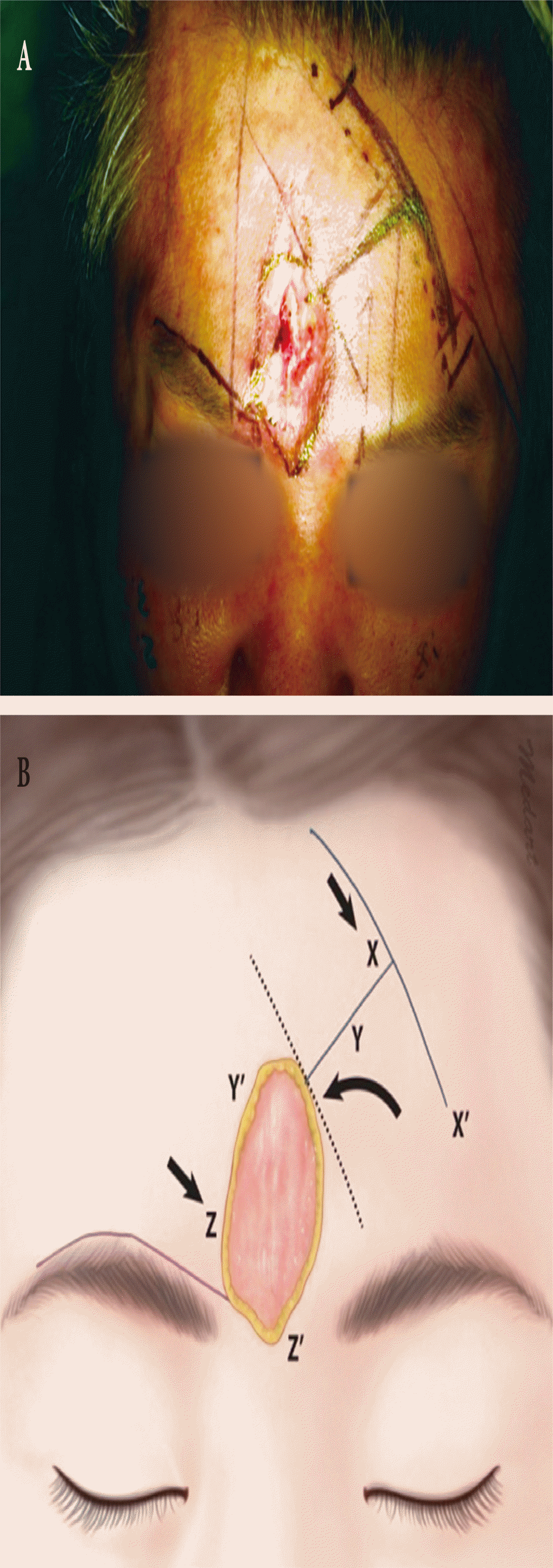
The patient underwent surgery under systemic anesthesia on day 1 of admission. To effectively cover the 3×4-cm2 midline forehead skin defect that was created after removing necrotic tissue and poorly healed granulation tissues, modified double-opposing rotation-advancement flaps were designed. After adequate debridement, the flaps were raised on the subgaleal plane. The upper area of the eyebrow was released while partially releasing the skin of the lower area. The elevated lower left flap was rotated to cover the defect, and the upper left and upper right flaps were advanced to the defect (Fig. 3).
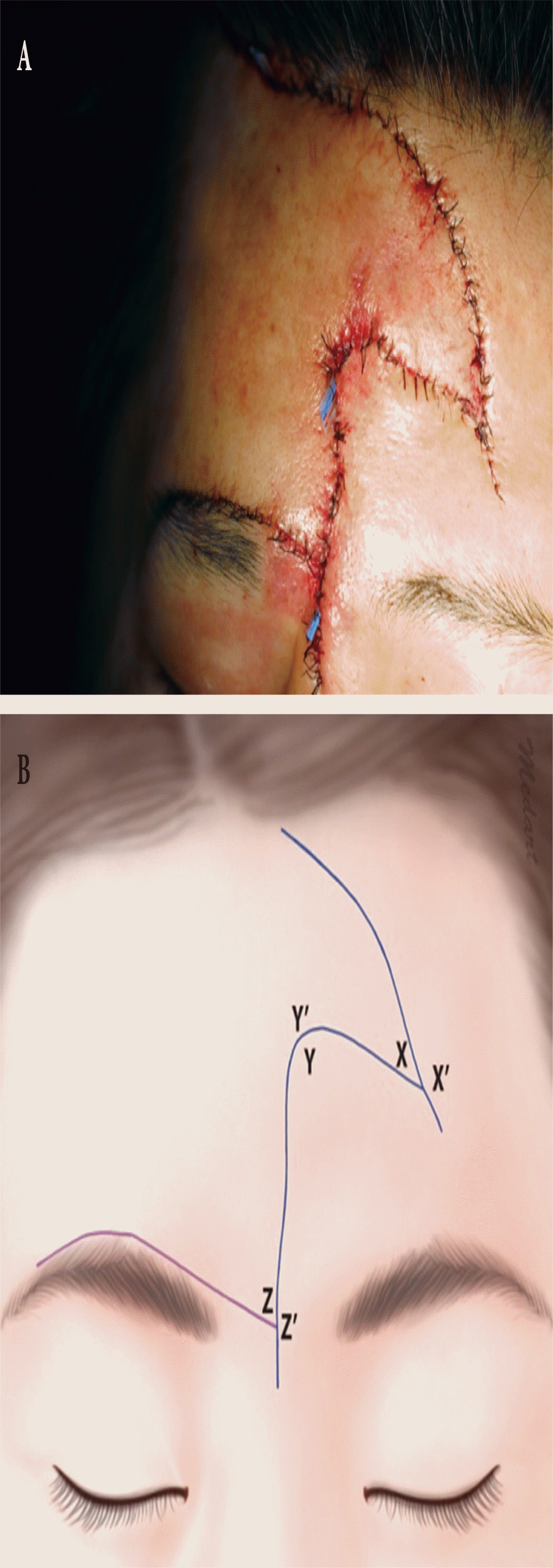
Suturing using absorbable polyfilament (Vicryl; Ethicon, Somerville, NJ, USA) with some pieces of fascia was performed in deeper skin layers. A second suture layer was placed on the epidermis using a nonabsorbable monofilament (Mersilk, Ethicon). Penrose drains were inserted (Fig. 4). There were no complications. The patient was discharged 10 days after surgery. It was confirmed that forehead reconstruction was successful at 3 months postoperatively (Fig. 5).
DISCUSSION
Vascular compromise after soft tissue augmentation with injectable facial fillers is a complication that should be addressed postoperatively. In particular, facial areas such as the glabellar area have been reported to be at higher risk for necrosis due to compromised blood flow attributable to the vascular anatomy of the area [5].
It has been reported that when filler-induced soft tissue necrosis is clinically suspected, various treatment approaches such as heparin, corticosteroid, hyaluronidase, platelet-rich plasma, and others are as effective as early interventions [5-7]. When necrosis has progressed past the acute phase, reconstructive surgery should be attempted.
The forehead is a facial region with distinct boundaries defined by the hairline superiorly, eyebrows and frontonasal groove inferiorly, and temporal ridges laterally. Therefore, reconstructing the region successfully without distorting the key landmarks is challenging [8]. Additionally, serious consideration should be given to midline forehead reconstruction to prevent eyebrow distortion (elevation of the medial eyebrows and medial displacement of the eyebrows) and to preserve motor and sensory nerve functions [9].
Regarding reconstruction of skin defects of the lower forehead or mid forehead near the glabellar area, Quatrano et al. [10] proposed that primary repair should be performed if the reconstruction area is smaller than 2 cm2, the modified Burow’s advancement f lap or A-to-T f lap should be used if the area is approximately 2–5 cm2, and a bilateral advancement flap or fullthickness skin graft should be used if the area is larger than 5 cm2. However, when full-thickness necrosis of the central mid-lower forehead skin occurs in an area as large as 10 cm2 (as in our patient), a bilateral advancement flap can distort the eyebrows, and a skin graft may lead to wound contraction, poor color, and mismatched texture.
Ransom and Jacono [4] presented the double-opposing rotation-advancement flap method modified from the orticochea flap method as a versatile reconstructive option for small, medium, and large forehead defects. However, there were limitations regarding eyebrow distortion and covering forehead defects larger than 10 cm2.
Accordingly, inspired by the double-opposing rotation-advancement flaps, we performed an additional incision along the superior border of the eyebrow contralateral to that used during the conventional approach. This unique flap design led to successful reconstruction because durable soft tissue covering a forehead skin defect as large as 10 cm2 was created during a single stage without altering the eyebrow position.
Although modified double-opposing rotation-advancement flaps have the disadvantage of leaving a longer scar compared to conventional approaches, the additional incision line made along the superior border of the eyebrow was camouflaged by the eyebrow. Therefore, it is believed that modified double-opposing rotation-advancement flaps are an excellent tool for central midlower forehead skin defect reconstruction.