Secondary Reconstruction of Frontal Sinus Fracture
Article information
Abstract
Fractures of frontal sinus account for 5%–12% of all fractures of facial skeleton. Inadequately treated frontal sinus injuries may result in malposition of sinus structures, as well as subsequent distortion of the overlying soft tissue. Such inappropriate treatment can result in aesthetic complaints (contour deformity) as well as medical complications (recurrent sinusitis, mucocele or mucopyocele, osteomyelitis of the frontal bone, meningitis, encephalitis, brain abscess or thrombosis of the cavernous sinus) with potentially fatal outcomes. Frontal contour deformity warrants surgical intervention. Although deformities should be corrected by the deficiency in tissue type, skin and soft tissue correction is considered better choice than bone surgery because of minimal invasiveness. Development of infection in the postoperative period requires all secondary operations to be delayed, pending the resolution of infectious symptoms. The anterior cranial fossa must be isolated from the nasal cavity to prevent infectious complications. Because most of the complications are related to infection, frontal sinus fractures require extensive surgical debridement and adequate restructuring of the anatomy. The authors suggest surgeons to be familiar with various methods of treatment available in the prevention and management of complications following frontal sinus fractures, which is helpful in making the proper decision for secondary frontal sinus fracture surgery.
INTRODUCTION
Fractures involving frontal sinus account for 5% to 12% of all fractures of facial skeleton [123456]. The frontal sinuses are pockets of space located above the orbit of each eye within the frontal bone. They are lined with mucous membrane, which secretes fluid that moistens and protects the nasal lining. The mucus drains through the infundibulum of the nasofronatal duct into the hiatus semilunaris and rest of the nasal cavity. The surgeon should be always aware of the obstruction of drainage system because this could make many complications. Due to the anatomic position of the frontal sinus and enormous amount of force required to create a fracture in this area, frontal bone fractures can be accompanied by concomitant injuries to the skull base, intracranial tissue, the orbital bones, and other facial bones.
Inadequately treated frontal sinus fractures may result in malposition of fractured segments as well as subsequent distortion of the overlying soft tissue. Such anatomical disruptions could result in contour deformity and also cause recurrent sinusitis, mucocele or mucopyocele, osteomyelitis of the frontal bone, meningitis, encephalitis, brain abscess or thrombosis of the cavernous sinus.
Proper management of frontal sinus fractures is all the more essential because of its proximity to vital structures, the brain. Despite this, the management of frontal sinus fractures remains controversial because postoperative complications can occur years to decades after the intervention. The consensus on posttraumatic frontal sinus reconstruction is that immediate treatment affords the best opportunity to restore the facial aesthetics, maintain the sinus function, and prevent many possible long-term risks of complications. Management options for frontal sinus fracture ranges from non-surgical treatment to open reduction and internal fixation with sinus conservation, and obliteration or cranialization of frontal sinus. In any given patient, the treatment modality should be based on the degree of fracture displacement, status of frontal sinus outflow tract, associated intracranial injuries. Depending on the institutional context, the patient may be cared by surgeons from a handful of specialties, such as otorhinolaryngologists, neurosurgeons, plastic or maxillafacial surgeons.
In this paper, we review the up-to-date literature regarding secondary reconstruction of frontal sinus fractures and assess the proper reconstructive options according to the cause of complications.
CLASSIFICATION OF FRONTAL SINUS FRACTURES
The primary treatment goal of facial injuries is to preserve both form and function. Therefore, treatment goals of the frontal sinus fracture are to maintaining sinus function, restoration of facial aesthetics, and prevention of complications.
Numerous classification schemes have been proposed of frontal sinus fracture [157891011]. Of all studies, a classification based on the involvement of frontal sinus outflow tract would best help to determine the treatment of frontal sinus fracture, from conservative treatment to operation [5]. However, the injury to the sinus outflow tract is not always easily detected on computed tomography (CT) scan, and the leakage of cerebrospinal fluid could be a cornerstone to determining treatment options [10]. Two major factors in considering treatment algorithm are patency of the frontonasal duct and persistence of the cerebrospinal fluid leaks. If the frontonasal duct is compromised, sinus obliteration or cranialization is required to prevent mucocele formation and infection.
Clinical features of frontal sinus fractures
Frontal sinus fractures are difficult to diagnose without radiologic studies, because the soft-tissue edema often obscures physical examination of the frontal bone. Signs suggestive of frontal sinus fracture include hypoesthesia of forehead and scalp, cerebrospinal rhinorrhea, subconjunctival ecchymosis, air in the orbit, depression over the forehead, or fractured bony fragments visible through an open wound [12].
All patients with severe head injury require high-resolution CT study for identification of intracranial injuries, which is more than adequate in assessing the frontal sinus. The presence of pneumocranium indicates posterior frontal sinus wall and/or skull base fracture, which is associated with significant intracranial hemorrhage in most cases (Fig. 1). This initial set of CT images are helpful not only in assessing the fracture itself but can also assist in medical decision making process and allows for comparisons to the postoperative CT scan. In addition, preoperative CT scans are helpful in identifying any injuries to frontonasal ducts [13].
The optimal method of treatment is determined by the site and extent of frontal sinus fracture. Accompanying facial bone fractures or brain injury could influence the treatment method as well as operation timing.
COMPLICATION AFTER FRONTAL SINUS FRACTURE TREATMENT
Complications after frontal sinus fracture treatment were subdived into aesthetic problems and infectious problem (Table 1).
SECONDARY TREATMENT OF COMPLICATIONS AFTER FRONTAL SINUS FRACTURE
Aesthetic problems
The frontal sinus fractures are typically the result of high-energy injuries with a force between 800 and 1,600 ft-lb. In addition to causing the fracture, the force can also damage the soft tissue and result in subsequent soft-tissue atrophy. The combination between fracture and soft-tissue atrophy explains the spectrum of aesthetic complications of frontal sinus fracture [1415]. In terms of contour, patients complain of forehead contour irregularity with protuberance or depression that causes washboard effect in the overlying soft tissue. Such deformities can occur for one or more of the following reasons: (1) failure to recognize that a displaced fragment will result in bony depression once the overlying soft tissue edema resolves; (2) inadequate realignment of displaced fragments; (3) overlying soft tissue atrophy by high energy injury; (4) elevation of a galeal flap that was used to address intracranial or cranial base injury; and (5) palpable metal plates and screws that were used for fixation of reduced frontal bone. It is important to note that contour deformity represents the most common cause of surgical "second look".
Bony framework is mainly affected by the adequacy of reduction. Kim et al. reported that contour deformity was rarely an issue for fractures whose posterior displacement was at or less than 4 mm. However, overlapped fractured edges may become palpable and become a source of postoperative complaint [16]. Forehead contour deformities can be managed by open reduction of displaced fracture, autologous bone graft from calvarium or pelvic bone, or onlay graft of alloplastic material. Irregularities based on mal-unioned bony base will require alloplastic or autogenous material or a combination of the two. Hydroxyapatite cement is useful when the deformity is scattered and depressed with concavity [17]. Also, Chen et al. [18] reported satisfactory outcomes following correction of frontal contour irregularities using hydroxyapatite cement and noted that the use of biocompatible alloplastic material was associated with stable volume maintenance. In fact, much of the recent literature on this topic seems to favor the use of alloplastic materials, such as hydroxyapatite and carbonated apatite, over the use of autologous bone graft for anterior table reconstruction [171819202122].
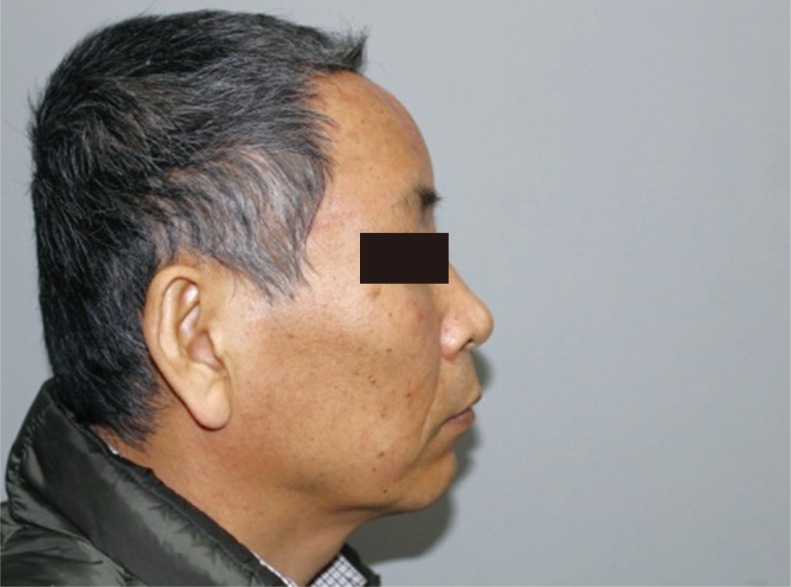
In addition to bony depressions, patients may suffer from scars or dimples over the forehead. Such changes to skin texture may develop as a result of laceration, abrasion, surgical incision, or from adhesions between skin-soft tissue envelope and underlying structures. Depressions limited to soft tissue could be treated by filler injection or fat grafting [23]. Fat grafting has many advantages over filler injection because it is autologous and semipermanent. Moderate scarring of soft tissue could be treated fat graft with V-dissector that could release scar contracture. Fat graft alone may not be adequate in addressing soft-tissue problems arising from severe scarring of soft tissue. Dermofat graft could be an alternative to release severe depression with scarring. It is especially useful when previous operative skin scar was noted. However, if there were no previous scar near the depression site, the use of dermofat is limited because surgeon should made new incision to inset the dermofat (Figs. 2, 3).

In this patient with craniectomy and cranioplasty with Medpor, the right forehead has a conspicuous scar with depressed contour.
Infectious problem
Posttraumatic and postoperative infections are more common for patients with multiple fractures or complex fractures than for patients with simple isolated fractures. The highest incidence is found with open fractures from penetrating trauma. Also, the risk of infection is higher for those fractures with concomitant maxillofacial injuries, possibly due to greater bone and mucosal destruction [242526].
In physiologic state, the ciliated sinus epithelium transports the secreted mucus through the nasofrontal duct into the nasal cavity. Preserving this drainage system has been the main goal in the management of frontal sinus fractures. Treatment options include observation, endoscopic drainage, open reduction and internal fixation of the frontal sinus anterior wall, maintenance of sinus function preserving the continuity of nasofrontal duct drainage, and sinus obliteration (with a broad range of matters). Some complicated cases of frontal sinus fractures may require sinus cranialization; however, the benefit of cranialization was controversal [27]. Clinical and experimental evidence suggest that duct obstruction and/or remnant sinus mucosa due to inadequate obliteration are serious predisposing factors of infectious complications [28].
Sinusitis
Frontal sinusitis, with or without gross purulence, usually results from intermittent obstruction of the nasofrontal drainage system. After frontal sinus injury, the frontal sinus can drains through venules known as the foramina of Breschet into the dural veins, allowing for intracranial spread of pathogens. Debate surrounds the use of prophylactic antibiotics, especially beyond the perioperative period with a large meta-analysis failing to show a significant decrease in the risk of meningitis and any other infectious complication [2930]. Such data must be weighted against the risk of severe opportunistic infections and selecting for resistant flora. Intractable frontal sinus infection can spread into the ethmoid sinus as well. Sinusitis with osteomyelitis should be addressed with adequate debridement, and the resulting dead space should be obliterated with a well-vascularized flap. The delay in necessary operation is one major risk factor for serious infection, and operations performed within 48 hours of injury is associated with the risk of severe infections [31]. Surgeons should not hesitate to operating on a patient with risk factors for infection, such as multiple fractures and CSF leakage.
The key to successful control of intractable infection is to seal the anterior skull base with sufficient volumes of a flap of well-vascularized tissue because vascularized tissue is believed to provide better protection against infection [32]. If the infection extends beyond the frontal sinus into the ethmoid sinus, both spaces should be obliterated. Adequate debridement of infected tissue is crucial to treat sinusitis. In these cases, local flaps may not be sufficient and require the use of a free muscular flap [32]. When the recipient vessel is injured or not available, reverse temporalis muscle flap could be a good alternative. Because this method provides a large arc of rotation and a relatively large volume of muscle, it could be also used for when severe soft tissue scarring make for a difficult galea or pericranial flap harvest [33].
Mucocele and mucopyocele
The most frequent complication from inadequate drainage of frontal sinus is mucocele. The frontal sinus mucosa can be tenacious, and inadequate drainage of mucus can manifest as a mucocele even though many years later [15]. A mucocele results from the regrowth of remnant mucosa and subsequent resumption of mucus production without a patent nasofrontal duct. Infected mucoceles are referred as mucopyocele or pyocele, which contains pus. Untreated frontal sinus fracture could made mucocele with the closure of the frontal sinus ostium by a block of bone after several years [34].
Clinically, symptoms of mucocele are benign in most cases [34]. Headache is the most common symptom, and other symptoms include proptosis, diplopia, nasal congestion, fluid leakage from the nose, and swelling over the forehead [35]. The anterior table is thick, whereas the posterior table is very thin. Therefore the mucoceles are expanded to posterior and inferior direction that made symptoms decribed above. In severe cases, strabismus may arise secondary to bilateral frontal sinus mucocele [36]. On CT images, a mucocele appears as a non-enhancing, low-attenuation expansile mass, and MRI studies show mucoceles as well-defined, expansile masses with variable signal intensities on T1 and T2 images [37].
Mucoceles that result from trauma are mostly due to compromised ventilation, and have been reported to occur between 1 and 35 years later in the literature [38]. Late appearance of mucoceles (or mucopyocele) remains always a possibility and, therefore, long-term clinical and computed tomography scanning follow-up have been suggested. Preventive cranialization of the frontal sinus to prevent secondary mucocele following frontal bone fracture is controversial [39].
Treatment of a mucocele consist of removing the mucocele sac and reestablishment of normal sinus drainage. Studies have reported success rates between 78% and 97% for external approaches, the Lynch and modified Lynch procedures, and osteoplastic flap techniques with or without frontal sinus obliteration [40]. The safest way to management a mucocele is to remove the sinus mucosa completely. Many surgeon perform a standard external approach combined with cranialization of the frontal sinus, meticulous eradication of the mucosa, and wide nasal drainage from the frontal base to the nasal cavity, and reconstructing the soft tissue and bony framework. Open approaches such as obliteration or cranialization have been shown to be effective in treating the problem, although recurrence rates have been reported to be as high as 25% [41]. In most cases, newly created extradural spaces become obliterated by the expansion of the frontal lobe within several weeks. In addition, vascularized local flaps, such as galeal frontalis, pericranial, or transverse glabellar, are highly effective in preventing contamination of the anterior cranial fossa from the paranasal space as vascularized option for sinus obliteration. The author prefers to use the galeal frontalis myofascial flap because of the following: (1) good vascular supply, (2) enough volume to fill the dead space of the frontal sinus, (3) narrow flap allows for greater degrees of rotation, (4) and short operation time [42]. This flap should be in the armamentarium of any surgeon faced with the task of sinus obliteration. However, when the mucocele is detected in an early stage, the treatment options of mucocele include minimally invasive approaches, which have considerably less morbidity.
Osteomyelitis of frontal bone
Osteomyelitis of frontal bone occurs because of severely comminuted, through-and-through frontal sinus fracture [43]. Chronic sinusitis could be a cause of osteomyelitis due to failed attempts at obliterating sinus mucosa and improper partitioning of the upper aerodigestive system from the anterior cranial base [4445]. Since the introduction of antibiotics, frontal bone osteomyelitis has become a uncommon complication. When osteomyelitis is present, however, antibiotic treatment is rarely effective because of the lack of blood supply to the necrotic bone and bone sequestra. It is important for the surgeon to review prior interventions to fully appreciate the extent of debridement needed and the availability of reconstructive plans. Once osteomyelitis has set-in, radical debridement is crucial to removal all necrotic dead tissue, foreign bodies, and hypertrophic granulation tissue with high bacterial counts. After proper debridement, the reconstruction could be performed with alloplastic or autologous materials.
Although numerous studies have reported using non-vascularized materials for sinus obliteration, the author is of the opinion that non-vascularized material itself can serve as a nidus for infection [4445]. It is generally accepted that well-vascularized tissues have greater ability to resist local soft-tissue infection and control osteomyelitis. Among various local flaps, the pedicled temporalis muscle myofascial flap has been demonstrated to be a useful and safe option in craniofacial reconstruction and for cranial base defects. The galea flap and pericranial flap is not recommended because these usually cannot provide sufficient volume [46]. The temporal muscle flap is most frequently used for laterally and antero-laterally located defects, although it can be mobilized across the midline [47]. Coverage of defect by local flaps have advantages of easier surgical technique, matching skin texture and thickness, shorter operation time, and less donor-site morbidity, when compared with free-tissue transfers. However, various free tissue transfer method have been described for reconstruction of forehead defects [474849505152]. Microvascular free flaps are superior to local flaps in providing a good sealing of the anterior cranial base, adequate filling up the dead space with a viable muscle and taking care that no virtual cavity was left behind. Free flaps also provide the benefit of enhanced circulation to overcome local infections, promoting rapid wound healing and skin revascularization [53]. The choice of most appropriate reconstruction depends on the location and size of the defect, type of tissue needed, and preferences of the surgeon.
Pott's puffy tumor
Pott's puffy tumor (PPT), first described by Sir Percivall Pott in 1760, is a rare clinical entity characterized by subperiosteal abscess associated with osteomyelitis. It is an osteomyelitis of the anterior wall of frontal bone commonly due to a frontal sinusitis (hematogenic spread) or, less commonly, due to frontal blunt trauma and frontal sinus reconstruction (direct translocation), of which the latter type of spread is limited to the adolescent age group [545556].
The tumor results in a swelling on the forehead, hence the name. The infection can spread inwards, leading to an epidural abscess, cortical vein thrombosis, subdural empyema, and brain abscess. Treatment of PPT generally consists of surgical drainage and long-term antibiotics.
Other infectious problem
Among frontal sinus fracture patients, delayed complications such as meningitis and encephalocele are very rare but are potentially life threatening [57]. Such complications require a multidisciplinary team that includes plastic surgery, neurologic surgery, otolaryngology, infectious disease, and critical care.
CONCLUSION
The frontal sinus is located the upper one-third of the facial skeleton. Frontal sinus fractures can result in a broad spectrum of complications, from forehead contour deformity to life-threatening infections. Therefore, each frontal sinus fracture patient should be informed to the possible complications and the importance of long-term follow up. Appropriate initial management is most important to minimize the risk of these complications.
Although contour deformity of forehead can be treated with various graft methods, fat grafting is a first line treatment because it is minimally invasive and simple. Autologous and alloplastic bone are indicated for moderate-to-severe bony displacement.
Almost every complications of frontal sinus fracture are related to infections. Extensive surgical debridement and adequate volume replacement are required to control these infections. The authors suggest surgeons to be familiar with various methods of treatment available in the prevention and management of complications following frontal sinus fractures, which is helpful in making the proper decision for secondary frontal sinus fracture surgery.
Notes
No potential conflict of interest relevant to this article was reported.