INTRODUCTION
Facial bone fractures are commonly seen in emergency medical care, and patients with severe facial fractures may present with massive bleeding. Most of these blooding can be controlled by suturing or temporary packing of the fracture site [1]. Persistent bleeding after packing or suturing is not common but is associated with high mortality rate. Although ligation of external carotid artery is an effective method to stop the bleeding in emergent time, it is associated with significant failure rate because of the collateral circulation of the carotid system. In such patients who continue to bleed after external means of hemostasis, emergency selective angiography should be considered early in the presentation. It can accurately identify the source of bleeding, and embolization of the bleeding branches can arrest the hemorrhage. The authors report a case of life-threatening hemorrhage from facial fracture.
CASE REPORT
A 73-year-old male commercial driver was involved in a motor vehicle accident with significant facial trauma. Out in the field, the patient was hypotensive and tachycardic (systolic blood pressure, 80 mm Hg; heart rate, 128), with an estimated hemorrhage of 1,000 mL. The patient was transported to our institution and bled an additional 100 mL in the initial 10 minutes of assessment. Physical examination revealed a left zygomaticomaxillary complex fracture injury with significant bleeding in the nasal and oral cavities, and the patient was actively resuscitated with fluids. Packing of the nasal and oral cavity was not effective in controlling the bleeding, and the patient was intubated to protect the airway.
After the initial fluid resuscitation with 2 liters of normal saline, the patient continued to have unstable vital signs and was transfused with 2 units of packed red cells, along with an additional liter of fluid. Despite vigorous resuscitation, the systolic pressure dropped further to 50 mm Hg. The initial laboratory study showed a hemoglobin level of 9.7. At this point, the patient's past medical history was not available, but the patient had been taking warfarin with a history of stroke three years prior to this.
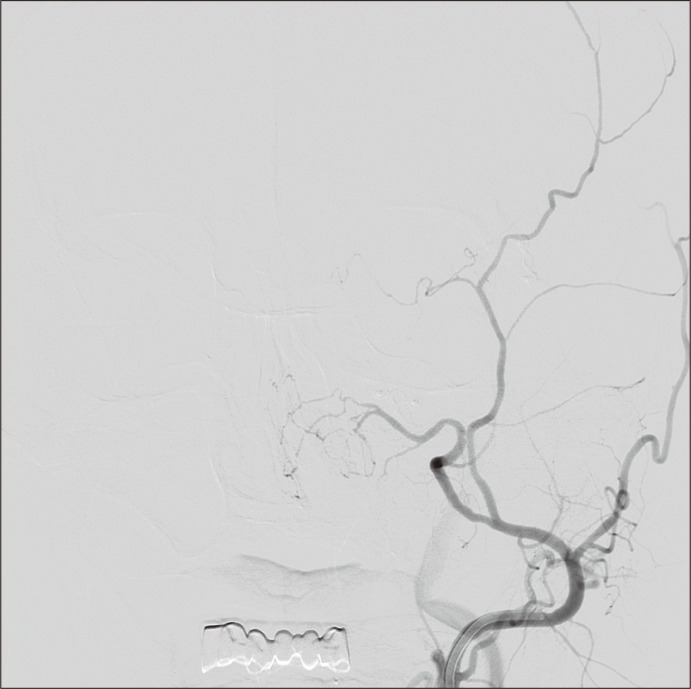
Computed tomography scan revealed a left zygomaticomaxillary complex fracture (Fig. 1). The patient was taken to the operating room for emergency reduction of the fracture with the primary goal of obtaining hemostasis. Upon exploration of the open wound in the oropharynx, the major source of bleeding was seen to originate from the left sphenopalatine fissure. During the 2-hour operation, the patient received an additional 3 units of packed red blood cells. Reduction of the facial skeleton was not sufficient in controlling the hemorrhage, and the patient was taken to the angiography suite. Angiogram of the external carotid artery revealed brisk extravasation of contrast from branches of the left sphenopalatine artery (Fig. 2). With embolization of this artery, the bleeding finally stopped, and the patient became hemodynamically stable without the need for further transfusion (Fig. 3). The patient was subsequently transported to the intensive care unit and recovered well enough to be extubated and transferred to the ward after 3 days. The patient was discharged home 3 months after the injury and returned to full employment.
DISCUSSION
Facial fractures are relatively common, and patients do not usually present with a life-threatening state. That occurs as a result life-threatening hemorrhage in facial fracture has become one of the important causes of death as contrary to many people's idea. Life-threatening hemorrhage occurs in 1% to 11% of patients with facial fractures [2]. Massive bleeding from facial fractures are rare but is associated high rates of mortality because of hypovolemic shock and airway obstruction [3]. Other life-threatening complications include arteriovenous fistula and carotid arterythrombosis [4].
The primary way to stop the bleeding includes suturing or applying pressure to the wound. Blind techniques, such as suturing or packing are indirect methods, which cannot directly access the origin of bleeding. Additionally, packing can result in complications such as mucosal excoriation and hypoxic damage. Failure with these initial measures represent one of two major problems. One potential problem is that the patient may be coagulopathic from excessive bleeding, or may have been taking anticoagulant medication [5]. The other potential problem is that the bleeding is originated from a location that is not accessible in emergency setting—the palatine and inferior alveolar arteries being the most difficult to control through non-angiographic means in such context [6]. To arrest massive bleeding from facial fracture, we pack the bleeding wound with epinephrine gauze and inject lidocaine/epinephrine (1:80,000) mixture around the posterior maxilla. Significant facial artery injuries require isolation and ligation of the disrupted vessel. At times, ligation of external carotid artery may not treat the origin of bleeding because of collateral circulation from both sides of the carotid complex.
If such massive bleeding cannot be controlled through surgical means, angiographic embolization should be considered sooner than later because these patients often require large amounts of transfusion just to maintain a life-sustaining cardiovascular function. Selective carotid angiography will locate the source and identify the extent of a bleeding, and embolization of the involved terminal branches can drastically alter the amount of transfusion required.
Transcatheter embolization has been widely used for the treatment of retroperitoneal bleeding. Embolization of branches of external carotid artery has been used for treatment of hypervascular tumours of face, as well as to stop severe epistaxis. In our patient, all attempts to control bleeding was unsuccessful until the arterial bleeding was stopped from within the vessel lumen. Published case reports indicate that transcatheter arterial embolization is being used more frequently to treat massive hemorrhage, with a reported success rate 87% [7]. Avascular necrosis is un-common following selective angiography and embolization of terminal branches of the external carotid artery. Postoperative surgical infection is uncommon in maxillofacial bone surgery. The reported incidence is less than 1% [8].
Massive hemorrhage from facial fractures may be an underrecognized clinical entity. Early recognition and proper management may reduce high mortality rate in this subset group of facial trauma patients. In patients with estimated blood loss greater than 500 mL, transcatheter arterial embolization is highly successful in saving the patient's life. Interhospital auditing and communication are recommended for optimizing institutional outcomes.