|
 |
- Search
| Arch Craniofac Surg > Volume 18(2); 2017 > Article |
|
Abstract
With advances in diagnostic technology, radiologic diagnostic methods have been used more frequently, and physical examination may be neglected. The authors report a case of pediatric medial orbital trapdoor fracture in which the surgery was delayed because computed tomography (CT) findings did not indicate bone displacement, incarceration of rectus muscle, or soft tissue herniation. A healthy 6-year-old boy was admitted to the emergency room for right eyebrow laceration. We could not check eyeball movement or diplopia, because the patient was irritable. Thus, we performed facial CT under sedation, but there was normal CT finding. Seven days later, the patient visited our hospital due to persistent nausea and dizziness. We were able to perform a physical examination this time. Lateral gaze of right eye was limited. CT still did not show any findings suggestive of fracture, but we decided to perform exploratory surgery. We performed exploration, and found no bone displacement, but discovered entrapped soft tissue. We returned the soft tissue to its original position. The patient fully recovered six weeks later. To enable early detection and treatment, thorough physical examination and CT reading are especially needed when the patient shows poor compliance, and frequent follow-up observations are also necessary.
Laceration and facial bone fracture can easily occur after blunt trauma to the periocular area. Occasionally, it is difficult to perform an accurate physical examination on pediatric patients with facial trauma, because they are irritable or unable to express their symptoms, which leads to poor compliance. In such cases, a fracture is diagnosed based on radiologic findings, such as X-ray or computed tomographic (CT) finding.
Trapdoor type fractures are more frequent in pediatric orbital wall fractures than in orbital wall fractures in adults. Pediatric orbital trapdoor fracture is often overlooked, as it is commonly accompanied by lack of external signs of trauma, and radiologic evidence may be minimal [1]. Especially, trapdoor fracture can be neglected in medial wall fractures because most trapdoor fractures occur in the orbital floor [2].
In reported cases of pediatric medial orbital wall trapdoor fracture, there was no significant bone displacement, but soft tissue herniation or rectus muscle incarceration were observed in most of cases [1,2,3]. The authors report a case of pediatric medial orbital trapdoor fracture in which the surgery was delayed because CT findings did not indicate any evidence of a medial orbital wall fracture.
A healthy 6-year-old boy presented at our emergency room due to right facial injury suffered while riding a bicycle. At this presentation, the patient did not complain of nausea or vomiting. Physical examination showed a 4 cm-size laceration in the right eyebrow and right periocular swelling. Physical examination for eyeball movement or diplopia was not possible because the patient was sensitive to pain and irritable. Thus, CT was performed with 2 mm slice thickness under sedation to determine the presence of a fracture; neither bone displacement, muscle incarceration, nor soft tissue entrapment were evident on CT images (Fig. 1A, B). Primary repair of the laceration was performed while maintaining sedation, and after the procedure, the patient was returned home.
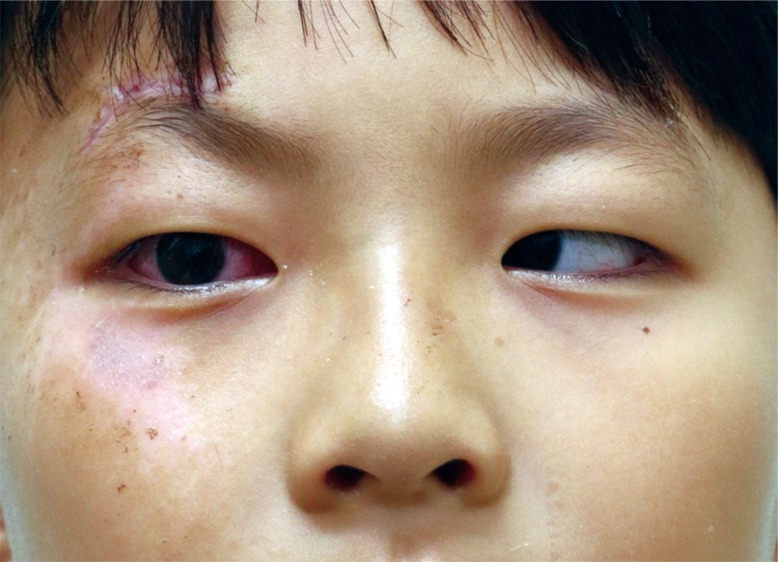
Seven days later, the patient visited a different hospital due to persistent nausea and dizziness, and was referred to our hospital for a thorough check-up. On this occasion, we were able to perform a physical examination, as pain and swelling had subsided. As severe limitation of extraocular movement and complete immobilization toward lateral gaze of the right eye were observed (Fig. 2). Rechecked CT images continued to show no evidence suggestive of fracture (Fig. 1C, D). Nevertheless, we decided to undertake exploratory surgery.
Forced duction testing under general anesthesia clearly showed abduction restriction in the right eye. A transcaruncular approach to the medial wall revealed no bone displacement, but did reveal entrapped soft tissue in the fracture line. This entrapped soft tissue was returned to its original position and surgery was concluded. The patient fully recovered six weeks later (Fig. 3).
Intense trauma to the periocular area induces a linear fracture line, and periorbital tissue tends to slip into the sinus and become entrapped when the bone fragment recoils to its original position. Soll and Poley [4] first referred to this phenomenon as âtrapdoor fractureâ. Large and comminuted fractures are more common in adults [5], whereas trapdoor fractures accompanied by soft tissue or muscle entrapment are more common in pediatric patients, because the facial bones of children are flexible and elastic due to incomplete mineralization [2].
Symptoms of trapdoor fracture include diplopia and pain, and a patient can occasionally display vagal symptoms (oculocardiac reflex), such as nausea, vomiting, bradycardia, and syncope [3,6]. CT findings may show herniated periocular tissue and incarcerated rectus muscle accompanying a linear fracture line.
Although the medial wall is the thinnest, fracture occurs most commonly in the floor because of the perpendicular partitions of ethmoidal air cells below the medial wall [7]. In floor fractures, rectus muscles are vulnerable to fracture, because there is no extraconal periorbital fat to act as a protective buffer. Like floor fractures, the medial wall also lacks a fat buffer, thereby increasing the high risk of muscle injury [3]. McCulley et al. [1] suggested that although medial rectus muscle incarceration was rare in trapdoor fracture as compared with inferior rectus muscle incarceration, they exhibit similar clinical manifestations.
Prompt surgical treatment is commonly recommended after an injury. However, there is a lack of consensus regarding the duration of surgical delay [5,8,9,10]. Yang et al. [2] suggested that patients could still recover to full extraocular movement when surgery is delayed by more than 72 hours, and thus, it would appear appropriate surgical techniques are also important predictors of fracture outcomes.
Pediatric patients with injuries to the facial area often display poor compliance due to pain and fear and an inability to express their symptoms adequately. In particular, compliance is even poorer when a trapdoor fracture is present, as it is frequently accompanied by oculocardiac reflex (nausea, vomiting) [1]. For these reasons, accurate physical examinations are problematic and radiologic findings are relied on heavily to determine the presence of a fracture. However, in most cases, definite bone displacement was not visualized by CT, but soft tissue or muscle herniation were visualized by CT. Although rare, medial wall trapdoor fracture may occur, and thus, the medial wall also should be closely inspected on CT images. In our case, CT was performed 2 mm thick and CT was performed twice, but no evidence of fracture was found. However, soft tissue herniation was observed during the operation. It is thought that incarcerated soft tissue was present between CT slices. In pediatric patients with intense facial trauma, it may be helpful to perform thin slice CT.
To enable early detection and treatment, CT findings are important, but accurate physical examination is mandatory, especially when a patient shows poor compliance, and frequent follow-up observations are also necessary as symptom onsets may be delayed.
References
1. McCulley TJ, Yip CC, Kersten RC, Kulwin DR. Medial rectus muscle incarceration in pediatric medial orbital wall trapdoor fractures. Eur J Ophthalmol 2004;14:330-333. PMID: 15309979.


2. Yang JW, Woo JE, An JH. Surgical outcomes of orbital trapdoor fracture in children and adolescents. J Craniomaxillofac Surg 2015;43:444-447. PMID: 25773374.


3. Neinstein RM, Phillips JH, Forrest CR. Pediatric orbital floor trapdoor fractures: outcomes and CT-based morphologic assessment of the inferior rectus muscle. J Plast Reconstr Aesthet Surg 2012;65:869-874. PMID: 22459795.


4. Soll DB, Poley BJ. Trapdoor variety of blowout fracture of the orbital floor. Am J Ophthalmol 1965;60:269-272. PMID: 14333982.


5. Kwon JH, Moon JH, Kwon MS, Cho JH. The differences of blowout fracture of the inferior orbital wall between children and adults. Arch Otolaryngol Head Neck Surg 2005;131:723-727. PMID: 16103306.


6. Sires BS, Stanley RB Jr, Levine LM. Oculocardiac reflex caused by orbital floor trapdoor fracture: an indication for urgent repair. Arch Ophthalmol 1998;116:955-956. PMID: 9682717.

7. Stotland MA, Do NK. Pediatric orbital fractures. J Craniofac Surg 2011;22:1230-1235. PMID: 21772209.


8. Jordan DR, Allen LH, White J, Harvey J, Pashby R, Esmaeli B. Intervention within days for some orbital floor fractures: the white-eyed blowout. Ophthal Plast Reconstr Surg 1998;14:379-390.


9. Grant JH 3rd, Patrinely JR, Weiss AH, Kierney PC, Gruss JS. Trapdoor fracture of the orbit in a pediatric population. Plast Reconstr Surg 2002;109:482-489. PMID: 11818824.


10. Cobb AR, Jeelani NO, Ayliffe PR. Orbital fractures in children. Br J Oral Maxillofac Surg 2013;51:41-46. PMID: 22497691.


- TOOLS
-
METRICS

-
- 6 Crossref
- Scopus
- 4,360 View
- 103 Download
- Related articles in ACFS
-
Reduction of Trapdoor Type Orbital Floor Fracture with Absorbable Mesh.2005 October;6(2)