|
 |
- Search
| Arch Craniofac Surg > Volume 19(2); 2018 > Article |
|
Abstract
Mandibular defects lead to severe deformation and functional deficiency. Vascularized osteocutaneous tissue has been widely used to reconstruct the mandible. However, it is technically challenging to shape this type of grafts in such a manner that they resemble the configuration of the mandible. A 48-year-old female patient who underwent anterolateral thigh (ALT) flap coverage after a tongue cancer excision was diagnosed with a tumor recurrence during the follow-up. A wide excision mandibulectomy and mandibular reconstruction with an ALT flap and a titanium implant were performed. The prefabricated titanium implant was fixed to the condyle. Then, an ALT flap was harvested from the ipsilateral thigh and anastomosed. After confirming that the circulation of the flap was intact, the implant was fixed to the parasymphysis. On the radiograph taken after the surgery, the prosthesis was well positioned and overall facial shape was acceptable. There was no postoperative complication during the follow-up period, 1 year and 2 months. The prefabricated implant allows the restoration of facial symmetry without harvesting autologous bone and it is a safe and effective surgical option for mandibular reconstruction.
Mandibular defects lead to severe deformation and functional deficiency [1]. Recently, vascularized osteocutaneous tissue grafts have been widely used to reconstruct the mandible [2,3]. In this case, we used computer-assisted design to fabricate a titanium implant based on a three-dimensional (3D) computed tomography (CT) image of the patientâs preoperative facial bone. This fabrication technique provided an anatomically customized reconstruction material for the patient.
A 48-year-old female patient was presented with a history of a squamous cell carcinoma on the left floor of the mouth and was surgically treated with anterolateral thigh (ALT) flap coverage after wide excision. She was diagnosed with a tumor recurrence on the left mandible body during the follow-up. Patient was examined by a multidisciplinary team and offered a reconstruction option using a prosthetic implant.
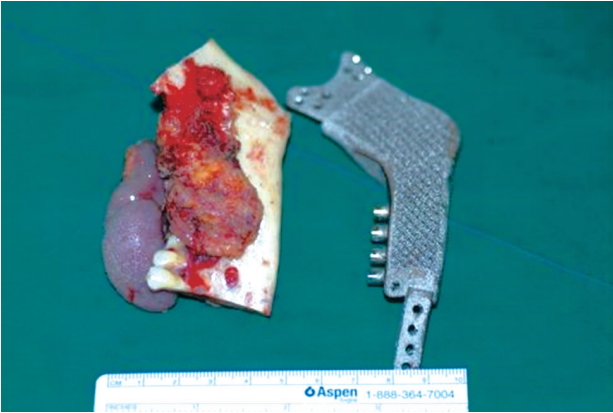
A 3D model of the facial bone was required to produce patientcustomized implants. In this case, we used two kinds of software to design the implant. A series of axial CT sections converted to 3D DICOM (Digital Imaging and Communications in Medicine) files and imported into MIMIC software (Materialise, Leuven, Belgium) [4]. The 3-matic software (Materialise) was used to build mesh arrays with geometries based on structural elements (Fig. 1) [4,5]. The designed implant was manufactured using an A1 metal 3D printer (Arcam, Molndal, Sweden) [6], with a biocompatibility material (Ti-6AL-4V-ELI medical grade powder) which is composed of titanium, aluminum, and vanadium [7].
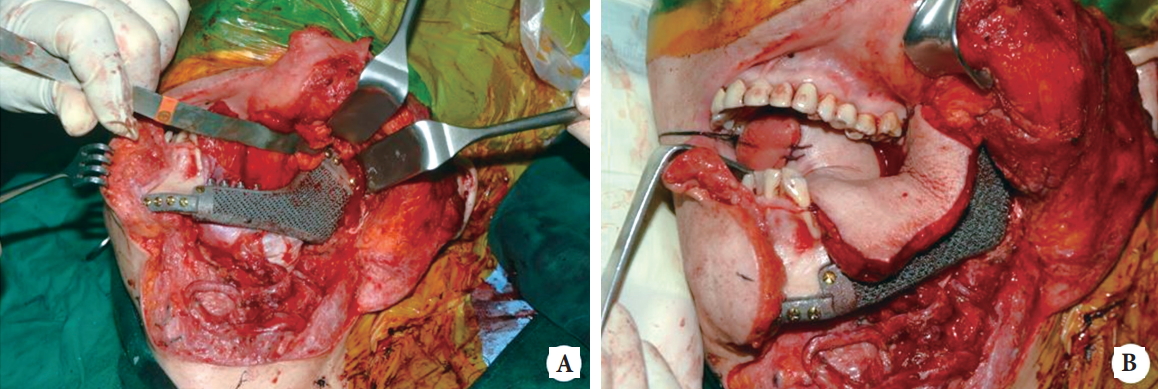
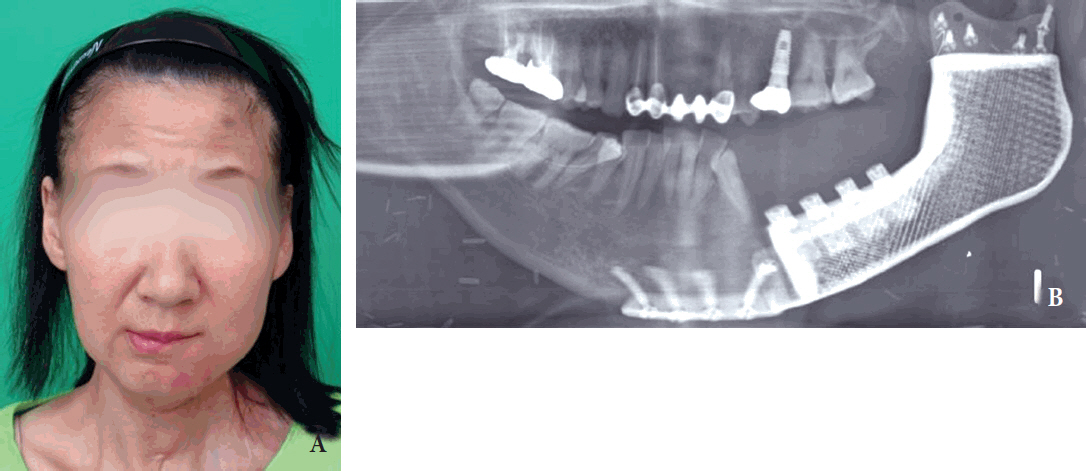
A wide excision and left mandibulectomy was performed followed immediately by a mandible, mouth floor, and tongue reconstruction with a titanium implant and an ALT free flap (Figs. 2, 3). As planned before surgery, the mandibulectomy created a large defect and a challenging reconstruction. First, the prefabricated titanium implant was fixed with a 2.4-mm screw to the condyle. Then, a 14Ă10-cm ALT flap was harvested from the ipsilateral thigh and anastomosed to the lingual artery and the internal jugular vein (Fig. 4). After confirming that the circulation of the flap was intact, the implant was fixed to the parasymphysis with a 2.4-mm screw. On the radiograph that was taken after surgery, the prosthesis appeared well positioned and the overall facial shape was acceptable (Fig. 5). The patient was capable of mastication and no suspicious tumor recurrence was observed on the follow-up CT. Due to the recurrence of the disease after the previous operation, the patient underwent adjuvant radiation and chemotherapy.
Bone defects in the mandibular region lead to severe deformation and impaired mastication, speech, swallowing, and respiration [8]. Mandibular reconstruction surgery is necessary not only to improve the appearance of the facial contour but also to improve the patientâs quality of life. In 1989, Jewer et al. [9] described a classification system for mandibular defects. According to Jewerâs HCL (H, hemimandibular; C, central; L, lateral) classification system, H defects are lateral defects that include the condyle, C defects involve the entire symphyseal area, and L defects are lateral defects that do not include the condyle.
Several treatment modalities have been developed to recover the original configuration of the mandible. In 1986, Gullane et al. [10] reported their use of myocutaneous flap in combination with stainless steel plate for restoration of mandibular defect following surgical resection. Nonvascularized bone grafts, such as those harvested from the iliac crest, have also been used [11,12]. However, the use of nonvascularized bone grafts is limited in the reconstruction of large defects or in cases where adjuvant radiotherapy is needed [13]. Recently, vascularized osteocutaneous grafts have been widely used to reconstruct the mandible. Bone grafts, such as a fibula free flap graft, can provide a sufficient amount of bone material to fill large mandibular defects [8]. Furthermore, a two-team surgical approach can be used when harvesting the vascularized fibula [14]. Most recently, computer-aided design and computer-aided manufacturing (CAD/CAM) techniques have been applied to mandibular reconstruction. By conducting a preoperative surgical simulation using the reconstruction plate as the surgical template, the accuracy of the reconstructive surgery can be improved [15].
Among the many surgical options, free vascularized osteocutaneous grafts have become the method of choice for most cases. However, there are some disadvantages associated with this technique. First, over the long-term, small amounts of bone graft volume loss can occur due to the absorption of the autologous tissue [12]. Second, there can be donor site morbidity due to the bone and soft tissue harvesting. Most graft sites are closed during the primary surgery but some may require additional skin grafts [16]. Third, because of the need for microsurgery, this type of graft is technically challenging and long operation times are required [8]. Fourth, it is difficult to shape the graft to resemble the original configuration of the mandible [8].
In the present case, we used individualized mandible implants that could be designed and fabricated in a relatively short time. The implants were fixed to the surrounding bone, provided a better fit, and covered a large defect. This study had the following limitations. This technique has not been applied to Jewerâs H defects that include the condyle. It also needs to be tested in the reconstruction of defects of the symphysis and the parasymphysis. Another limitation was that our long-term follow-up ended at 14 months. It might be necessary to observe the prosthesis for a longer period to confirm that it is well maintained.
In 2004, Schoen et al. [17] reported negative effects of radiation on osteointegration of dental implants. In addition, according to the study of Ryu et. al. [18] in 1995, in cases reconstructed with bridging titanium after mandibulectomy, the patients who received radiation therapy within 10 months after surgery had more loss of titanium plate than those who did not. However, it seems that there has been no definite study investigating the effect of radiation or chemotherapy on the prognosis after reconstruction with a prefabricated titanium implant in cases requiring mandibulectomy. As a result, in our case, adjuvant therapy seems to have no adverse effect on prosthesis or soft tissue flap during the follow-up period for 14 months.
The prefabricated implant allows the restoration of facial symmetry without harvesting autologous bone. To the best of our knowledge, this is the first reconstruction of the mandible with a titanium implant. We found this technique to be safe and effective with a shorter operation time, less donor site morbidity, and a better aesthetic outcome compared to a vascularized autologous reconstruction using the fibula, radius, and scapula.
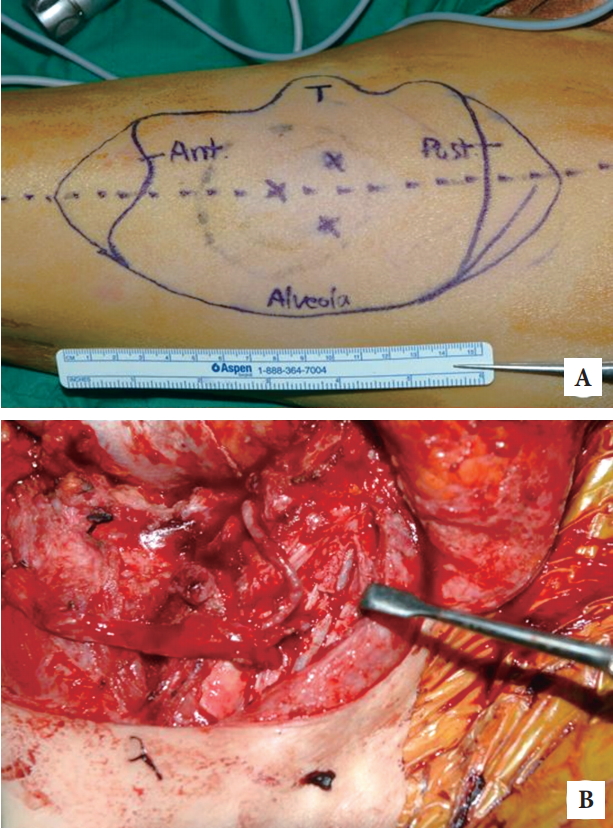
Fig. 3.
A design of the anterolateral thigh flap and vessels. A 14Ă10- cm anterolateral thigh flap was designed (A). The lingual artery and internal jugular vein were dissected as recipient vessels (B). Ant, anterior; T, tongue; Post, posterior.
REFERENCES
1. Singare S, Dichen L, Bingheng L, Yanpu L, Zhenyu G, Yaxiong L. Design and fabrication of custom mandible titanium tray based on rapid prototyping. Med Eng Phys 2004;26:671-6.


2. Cordeiro PG, Disa JJ, Hidalgo DA, Hu QY. Reconstruction of the mandible with osseous free flaps: a 10-year experience with 150 consecutive patients. Plast Reconstr Surg 1999;104:1314-20.


3. Spencer KR, Sizeland A, Taylor GI, Wiesenfeld D. The use of titanium mandibular reconstruction plates in patients with oral cancer. Int J Oral Maxillofac Surg 1999;28:288-90.


4. Qassemyar Q, Assouly N, Temam S, Kolb F. Use of a three-dimensional custom-made porous titanium prosthesis for mandibular body reconstruction. Int J Oral Maxillofac Surg 2017;46:1248-51.


5. Park EK, Lim JY, Yun IS, Kim JS, Woo SH, Kim DS, et al. Cranioplasty enhanced by three-dimensional printing: custom-made three-dimensional-printed titanium implants for skull defects. J Craniofac Surg 2016;27:943-9.


6. Rachmiel A, Shilo D, Blanc O, Emodi O. Reconstruction of complex mandibular defects using integrated dental custom-made titanium implants. Br J Oral Maxillofac Surg 2017;55:425-7.


7. Jo YY, Kim SG, Kim MK, Shin SH, Ahn J, Seok H. Mandibular reconstruction using a customized three-dimensional titanium implant applied on the lingual surface of the mandible. J Craniofac Surg 2018;29:415-9.


8. Zheng GS, Su YX, Liao GQ, Chen ZF, Wang L, Jiao PF, et al. Mandible reconstruction assisted by preoperative virtual surgical simulation. Oral Surg Oral Med Oral Pathol Oral Radiol 2012;113:604-11.


9. Jewer DD, Boyd JB, Manktelow RT, Zuker RM, Rosen IB, Gullane PJ, et al. Orofacial and mandibular reconstruction with the iliac crest free flap: a review of 60 cases and a new method of classification. Plast Reconstr Surg 1989;84:391-403.


10. Gullane PJ, Havas TE, Holmes HH. Mandibular reconstruction with metal plate and myocutaneous flap. Aust N Z J Surg 1986;56:701-6.


11. Pogrel MA, Podlesh S, Anthony JP, Alexander J. A comparison of vascularized and nonvascularized bone grafts for reconstruction of mandibular continuity defects. J Oral Maxillofac Surg 1997;55:1200-6.


12. Hidalgo DA, Pusic AL. Free-flap mandibular reconstruction: a 10-year follow-up study. Plast Reconstr Surg 2002;110:438-49.


13. Ndukwe KC, Aregbesola SB, Ikem IC, Ugboko VI, Adebiyi KE, Fatusi OA, et al. Reconstruction of mandibular defects using nonvascularized autogenous bone graft in Nigerians. Niger J Surg 2014;20:87-91.



14. Hidalgo DA. Fibula free flap: a new method of mandible reconstruction. Plast Reconstr Surg 1989;84:71-9.


15. Cohen A, Laviv A, Berman P, Nashef R, Abu-Tair J. Mandibular reconstruction using stereolithographic 3-dimensional printing modeling technology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2009;108:661-6.


16. Irish JC, Gullane PJ, Gilbert RW, Brown DH, Birt BD, Boyd JB. Primary mandibular reconstruction with the titanium hollow screw reconstruction plate: evaluation of 51 cases. Plast Reconstr Surg 1995;96:93-9.


- TOOLS
-
METRICS

-
- 13 Crossref
- Scopus
- 6,724 View
- 193 Download
- Related articles in ACFS
-
Anterior skull base reconstruction using an anterolateral thigh free flap2021 October;22(5)
Reconstruction of microstomia considering their functional status2020 June;21(3)