INTRODUCTION
A zygomaticomaxillary complex fracture is a common facial fracture. It is especially common in a high impact injury such as motor vehicle accident. Its clinical diagnosis is largely depending on computed tomography (CT). We have to differentiate maxillary fracture from many other events, including subcutaneous hematoma, maxillary sinusitis, and other facial fractures. Among them, maxillary sinusitis is a common disease encountered at the clinic. However, it is unusual in emergency room, even if it has unilateral presentation. A physician needs to be suspicious about unique mechanical causes that cause patientŌĆÖs symptoms, including tumor, fungi, or foreign bodies. Although foreign body in maxillary sinus is not a very rare finding, it can be confused with traumatic fracture at first.
In this report, we present a case of foreign body in maxillary sinus with impact 30 years ago, mimicking a maxillary fracture at first. This is a rare report of long-standing neglected foreign body in maxillary sinus. The foreign body was removed with endoscopic assistance.
CASE REPORT
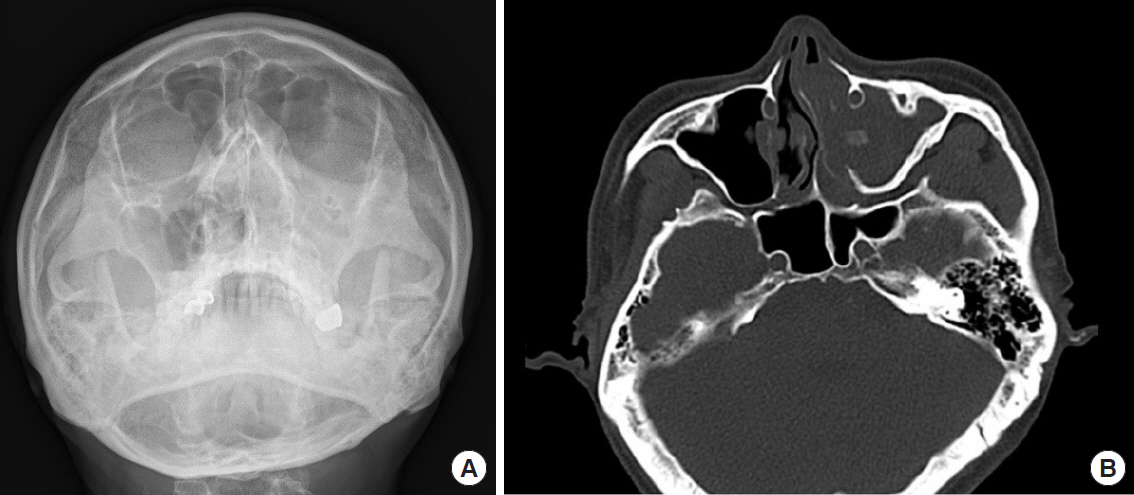
A 50-year-old systemically healthy male presented to the emergency department with a history of traffic accident and possible maxillary fracture. He complaint of mild degree of tenderness and numbness on his left malar area. He also had redness and swelling on his left cheek. Thus, we were suspicious of maxillary fracture. However, facial X-ray showed no visible displacement of zygomaticomaxillary complex. On the other hand, there was increase of haziness in maxillary sinus. Thus, CT was performed for more accurate evaluation. CT scan documented a large amount of fluid collection in left maxillary sinus without fracture line or broken bony structure (Fig. 1). There was a 4-cm long foreign body in maxillary sinus with the shape of a stick. After thorough history taking, we found a history of penetrating injury by chopstick about 30 years ago. He also felt bad smell in his nose and mouth sometimes.
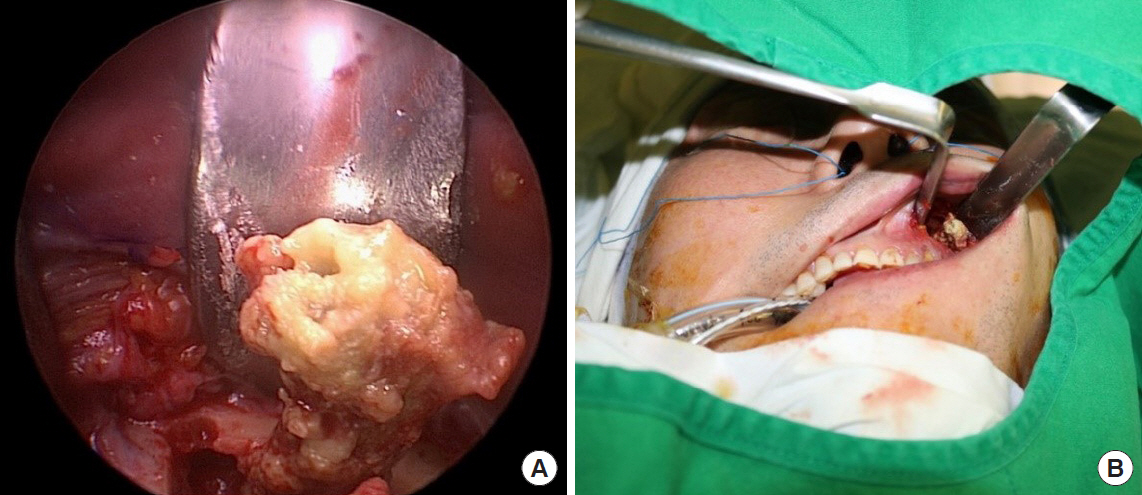
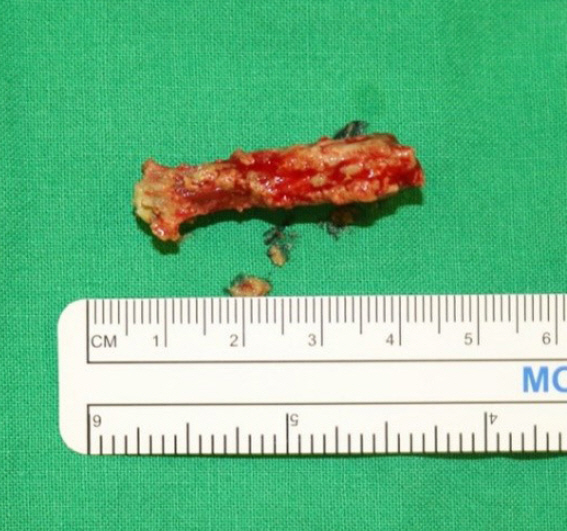
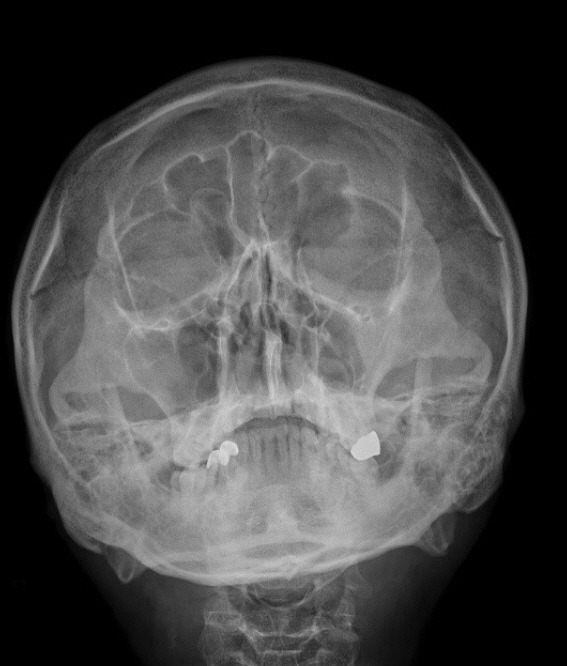
Under general anesthesia, gingivobuccal incision was made. Following mucoperiosteal flap elevation, the anterior bone wall of the maxillary sinus was revealed and a 20├Ś20 mm entry cavity for the endoscope was created by osteotomy. Once bleeding was under control, a sterilized endoscope was inserted into the sinus through this cavity. It was used to carefully remove the foreign body. The mucosa of the maxillary sinus was thickened and the sinus was filled with pus. The foreign body was coated with granulation tissues and debris (Fig. 2). It had the shape of a stick made of wood (Fig. 3). Surgical fields were irrigated with sterile saline and a pus was completely removed. After fixing the osteotomy site with miniplate, elevated flap was closed with Monocryl (Ethicon Inc., Somerville, NJ, USA) and Vicryl suture (Ethicon Inc.). After several days of admission with intravenous antibiotics, the patient was discharged without any problem. There were no complications following the operation up to 16 months of follow-up except persist numbness (Fig. 4).
DISCUSSION
The maxillary sinus is surrounded by a bony wall. It is a closed space. However, surgical treatment, trauma, and teeth as foreign bodies in the maxillary sinus have been reported. In our patient, CT images revealed a foreign body in the maxillary sinus. Nonmetallic foreign bodies are sometimes difficult to distinguish from a simple sinusitis on plain X-ray images. It has been reported that a wooden foreign body is not detected in CT scan. In that case, the foreign body was demonstrated as a radiolucent area like air [1]. Fortunately, CT images were useful to detect wooden foreign body in our case. However, we should notice radiolucent characteristic of organic foreign body and possibility of misdetection. When nonmetallic foreign body injury is suspected, we need to manipulate CT scanŌĆÖs slice interval or image demonstration setting.
Regarding treatment for foreign body, surgical removal is the treatment of choice. In our patient, CT images revealed that the foreign body was approximately 4-cm long. Since the mucosa of the maxillary sinus was thickened and the sinus was filled with pus, it was difficult to obtain a clear view of the surgical field using endoscope. Our anterior osteotomy helped us obtain direct operative vision and approach to the target area. Although target area could be reached with a trans-nasal endoscopic approach, this approach is insufficient to reach the bottom of the maxillary sinus because of its anatomical characteristics [2,3]. In our case, the foreign body size was too big to be removed from the nasal cavity. We also wanted to have a full range of surgical view from surgery to check the whole wall of sinus. Thus, we decided to take a transoral approach. We not only removed the foreign body easily, but also could assure that there was no fracture on the maxillary bone via this approach.
Foreign body induced carcinogenesis is a well-known biochemical reaction. This process is associated with prolonged repetitive irritation. In the process, many cytokines and free oxygen radicals can induce cytotoxic effects [4]. When an impacted foreign body is found, it should be removed immediately. When we found the foreign body, it was coated with granulation tissues and debris. We could not conclude when and where this stick was inserted into the maxillary sinus. However, based on interview with the patient and condition of the foreign body, the stick had been inserted in the maxillary sinus for at least several decades. We also performed pathological and microbiological evaluations. However, there was no malignancy or microbial infection.
A case of old foreign body mimicking nasal bone fracture has been reported [5]. In that report, a radiolucent plastic foreign body impacted subcutaneous tissue of nose. The author thought it was old-healed nasal bone fracture. Thus, open corrective rhinoplasty was performed. Foreign body impaction and facial bone fracture share history of high impact injury and painful swelling of injured area. If these are combined in a patient, it is difficult to distinguish the two. Thus, when foreign body penetration is highly suspicious, we should take thorough exploration and recommend CT scanning without any hesitation.