 |
 |
- Search
| Arch Craniofac Surg > Volume 22(6); 2021 > Article |
|
Abstract
Background
Methods
Results
Notes
Conflict of interest
Kwang Seog Kim and Jae Ha Hwang are editorial board member of the journal but were not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
Ethical approval
The study was approved by the Institutional Review Board of Chonnam National University Hospital (IRB No. CNUH-2021-342) and performed in accordance with the principles of the Declaration of Helsinki. Written informed consent was obtained.
Patient consent
The patient provided written informed consent for the publication and the use of his images.
Author contribution
Conceptualization: Kwang Seog Kim. Data curation: Seong Jin Oh, Jun Ho Choi. Formal analysis: Jae Ha Hwang, Sam Yong Lee. Methodology: Jae Ha Hwang, Sam Yong Lee. Project administration: Kwang Seog Kim. Writing - original draft: Seong Jin Oh, Kwang Seog Kim, Jun Ho Choi. Writing - review & editing: Kwang Seog Kim. Investigation: Seong Jin Oh, Jun Ho Choi.
Fig. 1.
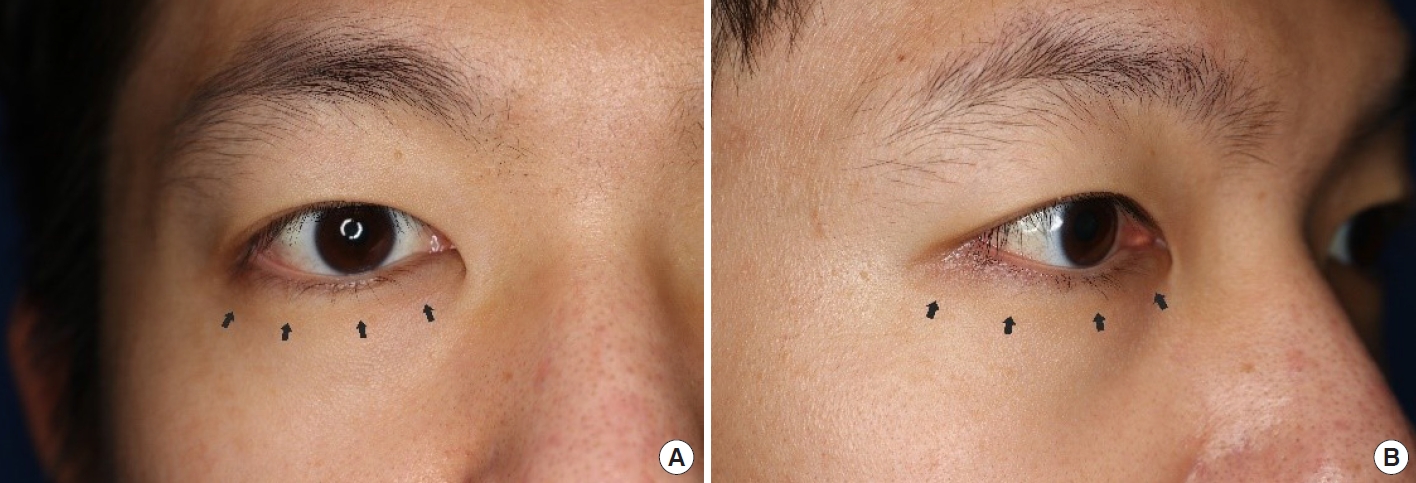
Fig. 2.

Fig. 3.
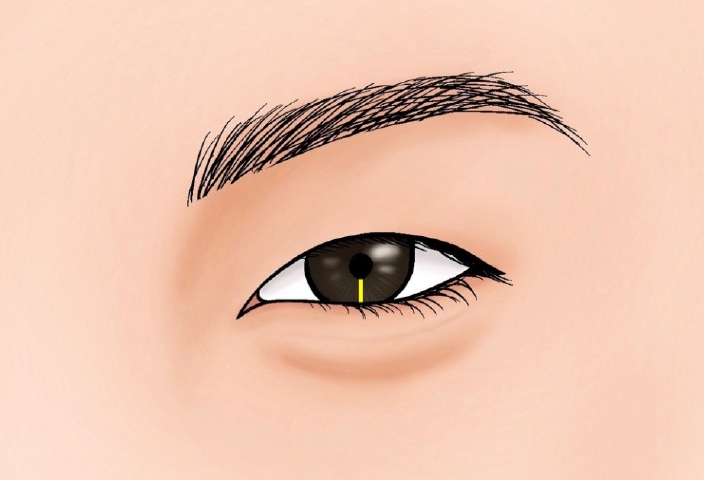
Fig. 4.
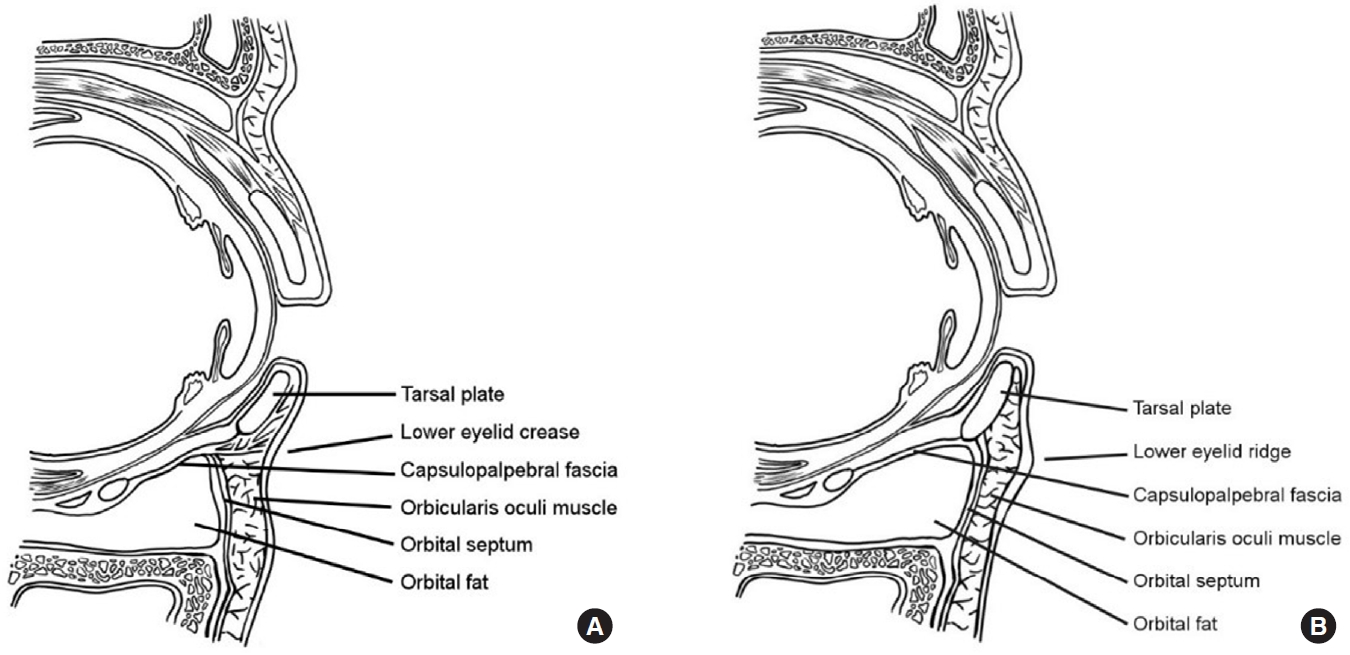
Table 1.
| Variable | Group A (n=23) | Group B (n=24) | Group C (n=13) | p-value |
|---|---|---|---|---|
| Age (yr) | 43.2±17.2 | 41.8 ± 13.8 | 34.1 ± 17.3 | 0.127 |
| Fracture type | 0.311 | |||
| Tripod fracture | 16 (69.6) | 14 (58.3) | 9 (69.2) | |
| Inferior orbital wall fracture | 3 (13.0) | 8 (33.3) | 4 (30.8) | |
| Both | 4 (17.4) | 2 (8.3) | 0 | |
| Fracture site | 0.918 | |||
| Medial | 4 (17.4) | 5 (20.8) | 4 (30.8) | |
| Central | 14 (60.9) | 15 (62.5) | 7 (53.8) | |
| Lateral | 5 (21.7) | 4 (16.7) | 2 (15.4) | |
| POSAS | 22.7 ± 8.0 | 20.9 ± 2.4 | 32.5 ± 4.1 | < 0.001a) |
| Group A:Group B | 0.548 | |||
| Group B:Group C | < 0.001a) | |||
| Group A:Group C | < 0.001a) | |||
| DMS (mm) | 2.4 ± 0.5 | 4.1 ± 0.7 | 5.8 ± 0.6 | < 0.001a) |
| DMCR (mm) | 5.22 ± 0.60 | 5.00 ± 0.59 | 4.77 ± 0.60 | 0.113 |
| DMPE widening | 0.001b) | |||
| No | 16 (69.6) | 24 (100) | 13 (100) | |
| Yes | 7 (30.4) | 0 | 0 | |
| Ectropion | ||||
| No | 23 (100) | 24 (100) | 13 (100) | |
| Yes | 0 | 0 | 0 | |
| Lateral extension scar | 0.795 | |||
| No | 19 (82.6) | 21 (87.5) | 12 (92.3) | |
| Yes | 4 (17.4) | 3 (12.5) | 1 (7.7) | |
| Follow-up (mo) | 8.09 ± 2.92 | 9.25 ± 3.05 | 7.85 ± 2.88 | 0.298 |
Values are presented as mean±SD or number (%). Group A, ≥ 2 mm above the lower eyelid crease or ridge; group B, within lower eyelid crease or ridge to 2 mm above the lower eyelid crease or ridge; group C, within lower eyelid crease or ridge to 2 mm below the lower eyelid crease or ridge.
POSAS, Patient and Observer Scar Assessment Scale; DMS, distance between the lower eyelid margin and the scar; DMCR, distance between the lower eyelid margin and the lower eyelid crease or ridge; DMPE, distance between the margins of the peripheral pupil and the lower eyelid.
Table 2.
| Group | DMCR (mm), mean ± SD | p-valuea) |
|---|---|---|
| Group A | 0.328 | |
| Fractured side | 5.22 ± 0.60 | |
| Normal side | 5.26 ± 0.62 | |
| Group B | 0.082 | |
| Fractured side | 5.00 ± 0.59 | |
| Normal side | 5.13 ± 0.68 | |
| Group C | 0.337 | |
| Fractured side | 4.77 ± 0.60 | |
| Normal side | 4.85 ± 0.69 |
Group A, ≥2 mm above the lower eyelid crease or ridge; group B, within lower eyelid crease or ridge to 2 mm above the lower eyelid crease or ridge; group C, within lower eyelid crease or ridge to 2 mm below the lower eyelid crease or ridge.
DMCR, distance between the lower eyelid margin and the lower eyelid crease or ridge.
Table 3.
| Variable | Group A (n = 23) | Group B (n = 24) | Group C (n = 13) | p-value |
|---|---|---|---|---|
| Observer component | ||||
| Vascularity | 1.3 ± 0.5 | 1.3 ± 0.5 | 1.5 ± 0.5 | 0.328 |
| Pigmentation | 1.1 ± 0.3 | 1.0 ± 0.2 | 1.3 ± 0.5 | 0.249 |
| Thickness | 1.7 ± 0.8 | 1.6 ± 0.5 | 1.7 ± 0.5 | 0.930 |
| Relief | 1.3 ± 0.4 | 1.1 ± 0.3 | 2.0 ± 0.4 | < 0.001a) |
| Pliability | 1.3 ± 0.5 | 1.2 ± 0.4 | 1.8 ± 0.4 | 0.006a) |
| Surface area | 1.5 ± 0.7 | 1.3 ± 0.5 | 1.6 ± 0.5 | 0.690 |
| Total score observer scar scale | 8.2 ± 2.3 | 7.5 ± 1.2 | 10.0 ± 1.2 | 0.025a) |
| Patient component | ||||
| Is the scar painful? | 1.3 ± 0.5 | 1.3 ± 0.6 | 1.6 ± 0.7 | 0.150 |
| Is the scar itching? | 1.8 ± 0.7 | 1.5 ± 0.6 | 1.8 ± 0.8 | 0.628 |
| Is the color of the scar different? | 2.2 ± 0.7 | 2.4 ± 0.7 | 3.9 ± 1.1 | < 0.001a) |
| Is the scar more stiff | 3.3 ± 2.0 | 2.8 ± 0.8 | 4.2 ± 2.0 | 0.270 |
| Is the thickness of the scar different? | 2.5 ± 1.1 | 2.8 ± 0.7 | 5.7 ± 1.3 | < 0.001a) |
| Is the scar irregular? | 3.3 ± 2.3 | 2.6 ± 0.8 | 5.3 ± 1.7 | 0.017a) |
| Total score patient scar scale | 14.5 ± 6.0 | 13.4 ± 2.0 | 22.5 ± 3.7 | < 0.001a) |
Values are presented as mean±SD. Group A, ≥ 2 mm above the lower eyelid crease or ridge; group B, within lower eyelid crease or ridge to 2 mm above the lower eyelid crease or ridge; group C, within lower eyelid crease or ridge to 2 mm below the lower eyelid crease or ridge.
POSAS, Patient and Observer Scar Assessment Scale.
Table 4.
| Variable | Coefficient (95% CI) | p-value |
|---|---|---|
| DMS | 2.40 (1.15 to 3.66) | < 0.001a) |
| Age | 0.07 (–0.04 to 0.18) | 0.186 |
| Follow-up | –0.12 (–0.68 to 0.44) | 0.674 |
| Lateral extension scar | 2.50 (–2.62 to 7.62) | 0.332 |
| Inferior orbital wall fracture | –1.32 (–5.57 to 2.92) | 0.534 |
| Tripod fracture and inferior orbital wall fracture | –2.18 (–8.04 to 3.68) | 0.459 |
Table 5.
| OR (95% CI) | p-value | |
|---|---|---|
| DMS | 0.14 (0.01–0.54) | 0.029a) |
| Age | 1.13 (1.03–1.33) | 0.048a) |
| Follow-up | 1.20 (0.79–1.93) | 0.392 |
| Lateral extension scar | 0.75 (0.04–12.01) | 0.841 |
Table 6.
| Variable | Group A (n = 16) | Group B (n = 24) | Group C (n = 13) | p-value |
|---|---|---|---|---|
| Age (yr) | 37.2 ± 16.8 | 41.8 ± 13.8 | 34.1 ± 17.3 | 0.660 |
| Fracture type | 0.541 | |||
| Tripod fracture | 10 (62.5) | 14 (58.3) | 9 (69.2) | |
| Inferior orbital wall fracture | 3 (18.8) | 8 (33.3) | 4 (30.8) | |
| Both | 3 (18.8) | 2 (8.3) | 0 | |
| Fracture site | 0.966 | |||
| Medial | 3 (18.8) | 5 (20.8) | 4 (30.8) | |
| Central | 10 (62.5) | 15 (62.5) | 7 (53.8) | |
| Lateral | 3 (18.8) | 4 (16.7) | 2 (15.4) | |
| POSAS | 17.7 ± 2.2 | 20.9 ± 2.4 | 32.5 ± 4.1 | < 0.001a) |
| Group A:Group B | 0.004a) | |||
| Group B:Group C | < 0.001a) | |||
| Group A:Group C | < 0.001a) | |||
| DMS (mm) | 2.5 ± 0.5 | 4.1 ± 0.7 | 5.8 ± 0.6 | < 0.001a) |
| DMCR (mm) | 5.12 ± 0.06 | 5.00 ± 0.59 | 4.77 ± 0.60 | 0.308 |
| DMPE widening | ||||
| No | 16 (100) | 24 (100) | 13 (100) | |
| Yes | 0 | 0 | 0 | |
| Ectropion | ||||
| No | 16 (100) | 24 (100) | 13 (100) | |
| Yes | 0 | 0 | 0 | |
| Lateral extension scar | 1.000 | |||
| No | 14 (87.5) | 21 (87.5) | 12 (92.3) | |
| Yes | 2 (12.5) | 3 (12.5) | 1 (7.7) | |
| Follow-up (mo) | 7.88 ± 2.87 | 9.25 ± 3.05 | 7.85 ± 2.88 | 0.263 |
Values are presented as mean±SD or number (%). Group A, ≥ 2 mm above the lower eyelid crease or ridge; group B, within lower eyelid crease or ridge to 2 mm above the lower eyelid crease or ridge; group C, within lower eyelid crease or ridge to 2 mm below the lower eyelid crease or ridge.
DMPE, distance between the margins of the peripheral pupil and the lower eyelid; POSAS, Patient and Observer Scar Assessment Scale; DMS, distance between the lower eyelid margin and the scar; DMCR, distance between the lower eyelid margin and the lower eyelid crease or ridge.
Table 7.
| Coefficient (95% CI) | p-value | |
|---|---|---|
| DMS | 3.97 (3.20 to 4.74) | < 0.001a) |
| Age | –0.04 (–0.11 to 0.02) | 0.207 |
| Follow-up | –0.12 (–0.46 to 0.22) | 0.407 |
| Lateral extension scar | 0.39 (–2.87 to 3.65) | 0.810 |
| Inferior orbital wall fracture | –1.05 (–3.47 to 1.37) | 0.387 |
| Tripod fracture and inferior orbital wall fracture | –1.76 (–5.40 to 1.87) | 0.334 |
REFERENCES
- TOOLS
-
METRICS

-
- 3 Crossref
- Scopus
- 3,956 View
- 106 Download
- Related articles in ACFS






