 |
 |
- Search
| Arch Craniofac Surg > Volume 23(1); 2022 > Article |
|
Abstract
Background
Intermaxillary fixation (IMF) is a technique that allows for the reduction and stabilization of mandibular fractures. Several methods of IMF, such as self-tapping screws or arch bars, have been developed. This study aimed to validate the usefulness of IMF with a self-tapping screw compared to IMF with arch bars with focus on the patients’ perspective.
Methods
We retrospectively reviewed the medical records of all patients who were treated for mandibular fractures at our hospital between August 2014 and February 2021. A total of 57 patients were enrolled in this study. Thirteen patients were excluded from the analysis: three patients were lost to follow-up, and 10 patients did not undergo IMF. Finally, 44 patients were analyzed, of which 31 belonged to the arch bar group, and 13 belonged to the screw group. Patient discomfort and pain during IMF application and removal were analyzed using a patient self-assessment questionnaire. The surgeon also assessed oral hygiene, IMF stability, and occlusion.
Results
We applied IMF to 34 men (77%) and 10 women (23%). The mean age of the patients was 37.3 years. The most common fracture site was the angle (30%), followed by the parasymphysis (25%), the body (23%), the condyle (11%), and the ramus (11%). Patient discomfort and oral hygiene were statistically favorable in the screw group. The IMF application time was statistically shorter in the screw group (p<0.001). IMF stability was not statistically different between the two groups. The pain score during IMF removal was lower in the screw group (p<0.001).
The mandible is a movable, predominantly U-shaped bone comprising horizontal and vertical segments [1]. Plastic surgeons in craniofacial trauma centers regularly encounter mandible fractures [2,3]. Several studies have investigated mandibular fractures; however, therapeutic strategies often depend on the surgeon’s experience and preference [4].
In patients with mandibular fractures, intermaxillary fixation (IMF) is used to restore dental occlusion and support [1]. In selected cases, IMF alone is the primary treatment modality (closed treatment) without open reduction and internal fixation (ORIF). However, if ORIF is required, IMF can be applied preoperatively to support internal fixation and for postoperative splinting [5,6].
Erich’s arch bar is a conventional method for IMF that securely holds both jaws and provides adequate traction. However, performing IMF using an arch bar is time-consuming and can cause gingival damage during fixation. In addition, several studies have pointed out that oral hygiene is relatively poor while maintaining arch bars [7].
The IMF using screws was developed as an alternative to arch bars in the 1980s. After applying 4–8 self-tapping screws in the maxilla and mandible near the mucogingival junction, IMF is achieved by fixing them with wires or rubber bands [7]. Thus, the operation time is shortened, and the possibility of gingival damage is reduced.
This study was designed to examine the differences between the two methods, especially from the patients’ perspective. We investigated patients who underwent IMF for patient comfort, oral hygiene, IMF stability, occlusion, and pain during IMF application and removal.
We conducted a retrospective chart review of patients diagnosed with mandibular fractures who underwent surgery between August 2014 and February 2021. In the analysis, we excluded unconscious patients and those who were lost to follow-up. Patients who underwent IMF were divided into two groups: IMF using arch bars and IMF using screws. This study was approved by the Institutional Review Board of Haeundae Paik Hospital (HPIRB 2021-06-005) and performed in accordance with the principles of the Declaration of Helsinki. The requirement for written informed consent was waived. All patients provided written informed consent for the publication and use of their images.
Arch bar application was performed under local or general anesthesia. Arch bars with hooks were applied to the external surface of the dental arch. Arch bars were fixed by passing 24-gauge steel wires through the necks of the teeth and twisting them around the teeth to hold the arch bars securely against the dental arch (Fig. 1A) [7].
IMF screw application was performed under general anesthesia, before or after ORIF, and self-tapping IMF screws of 2 mm diameter and 10–12 mm length were applied. A total of 4–8 IMF screws were applied (1) between the lateral incisor and canine (2) between the first and second premolars at the mucogingival junction (Fig. 1B). For the prevention of the root injury of the adjacent teeth, it is important to place the screws between the tooth roots and insert them perpendicularly. The surgeon adjusted the number and positions of the IMF screws according to the type and location of the fracture in order to provide appropriate vectors to restore occlusion (Fig. 2).
The time taken for IMF application was recorded. In addition, the patient indicated the severity of pain on a pain scale when IMF application was performed under local anesthesia. IMF was applied for 4–6 weeks. If the IMF needed to be maintained for an extended period, the arch bar was used.
IMF removal was performed on an outpatient basis under local anesthesia. At the time of IMF removal, the patient was administered a questionnaire. Comfort during the IMF maintenance period and pain during IMF removal were evaluated. The surgeon also assessed IMF stability, oral hygiene, and occlusion (Fig. 3).
Categorical variables between the two groups were compared using Fisher exact test. Continuous variables were compared between the two groups using the Mann-Whitney U test. Statistical significance was set at p<0.05. All analyses were performed using IBM SPSS Statistics for Windows version 25.0 (IBM Corp., Armonk, NY, USA).
A total of 57 patients were treated for mandibular fractures, of which three were excluded from the analysis because they were unconscious or lost to follow-up. Ten patients were excluded from the study because they underwent only ORIF without IMF. A total of 44 patients underwent IMF; 31 underwent arch bar application and 13 underwent IMF screw application.
Of the 44 patients analyzed, 34 were men, and 10 were women. Patient age ranged between 13 and 83 years, and the mean age was 37.3 years. The most common fracture site was the angle (30%). The other fracture sites included the parasymphysis (25%), the body (23%), the condyle (11%), and the ramus (11%). Road traffic accidents were the most common etiology of mandibular fractures (29.5%), followed by human assault (27.3%), slipping (25.0%), falling objects (6.8%), blast injuries (6.8%), and falls (4.5%).
The average time required for IMF application was 15.38 minutes in the IMF screw group and 52.41 minutes in the arch bar group (p<0.001). This finding shows a statistically significant reduction in the IMF application time when using IMF screws (Table 1, Fig. 4).
Fifteen patients underwent arch bar application under local anesthesia, and their average IMF application pain score was 6.60± 0.74. However, because all patients in the screw group underwent IMF application under general anesthesia, pain during screw application could not be evaluated in this group. All patients underwent IMF removal under local anesthesia. During IMF removal, the average pain score in the screw group was 3.69, whereas that in the arch bar group was 5.71 (Table 1), and the difference was statistically significant (p<0.001). This finding showed that patients who are treated with IMF using screws experience less pain during device removal as compared to the group using arch bar fixation.
We also assessed patients’ comfort during IMF at the time of IMF removal. In the IMF screw group, 11 patients (84.6%) reported endurable pain during the IMF period, while in the arch bar group, only 14 patients (45.2%) reported tolerable pain, and the difference was statistically significant (p=0.017) (Table 2).
The surgeon assessed the oral hygiene, occlusion, and IMF stability at the time of IMF removal on an outpatient basis. In the IMF screw group, 12 patients (92.3%) had adequate oral hygiene, while in the arch bar group, 16 patients (51.6%) had acceptable oral hygiene. The oral hygiene status was significantly favorable in the IMF screw group (p=0.015). Regarding IMF stability, in the IMF screw group, three patients (23.1%) had inadequate IMF stability, and in the arch bar group, eight patients (25.8%) had inadequate IMF stability. However, there were no statistically significant differences between the two groups (p=0.585). Malocclusion occurred in one patient (7.7%) in the IMF screw group and one patient (4.5%) in the arch bar group. There was no statistically significant difference between the two groups (p=0.508) (Table 2).
IMF plays an important role in the treatment of mandibular fractures. However, patients experience discomfort during the IMF period. Therefore, this study was designed to investigate patients’ experiences according to the type of IMF.
It is challenging to manage oral hygiene while maintaining IMF using an arch bar. Patients were instructed to maintain oral hygiene by performing saline gargles and using a Waterpik; however, oral hygiene was inadequate in patients with poor compliance. Patients belonging to the IMF screw group had better oral hygiene than the arch bar group. This is probably because the patients in the IMF screw group had fewer IMF components in the oral cavity, making it easy to cleanse the teeth and gingiva.
Regarding patient discomfort, patients experienced pain due to gingival or mucosal injury with sharply cut wires, which fixed the arch bar to the teeth. In addition, the wires or rubber bands fixing the arch bars of both jaws may irritate the oral mucosa. However, in the IMF screw group, only 4–8 screws were applied, and since they had a relatively blunt tip, they were less likely to cause discomfort and irritation to the buccal mucosa.
The surgeon preferred the arch bar when used alone for closed treatment. IMF using screws was usually applied with ORIF. Screws were preferred when surgery was performed immediately after an injury. In addition, patients with poor periodontal conditions were treated with screws.
Screw loosening in the IMF screw group occurred in three cases (23.1%), and we could handle it by tightening the screws at the outpatient clinic. In this study, no tooth root injury was observed in patients who underwent IMF screw fixation. When mucosal growth was seen over time, it could be resolved simply by stab incision under local anesthesia. In the arch bar group, arch bar loosening occurred in eight patients (25.8%), and we resolved this problem by tightening the wire again or removing and replacing the loosened wire. The loosening of the arch bar may be related to improper tightening of the wires, which is usually performed by residents.
Malocclusion is a common complication of mandibular fractures [8]. In this study, malocclusion occurred in one patient (4.5%) in the arch bar group and one patient (7.7%) in the IMF screw group. There was no significant difference in the incidence of malocclusion between the two groups. Both groups achieved satisfactory restoration of occlusion. Patients with malocclusion were later referred for orthodontic treatment.
In this study, we showed that the time needed for device application is reduced by approximately 70.7% in the screws group as compared to the arch bar group. Moreover, when used under general anesthesia, achieving IMF using screws can reduce the potential harm to the patient by decreasing the duration of anesthesia. However, the limitations of this study were its retrospective nature, and the absence of randomization of the patient groups. Moreover, the use of IMF screws is not recommended in all cases. IMF screws may not be appropriate if the patient has osteoporosis or if the fracture is severely comminuted.
In conclusion, IMF screws reduce the IMF application time and reduce patient discomfort. In addition, IMF using screws helps in maintaining good oral hygiene during the IMF period. Except for patients with osteoporosis or severely comminuted fractures, IMF application using screws is a better option from the patient’s perspective when performing ORIF a few days after injury.
Notes
Ethical approval
The study was approved by the Institutional Review Board of Haeundae Paik Hospital (IRB No. HPIRB 2021-06-005) and performed in accordance with the principles of the Declaration of Helsinki. The requirement for written informed consent was waived.
Patient consent
The patient provided written informed consent for the publication and the use of his images.
Author contribution
Conceptualization: Sung Ho Yoon, Keun Cheol Lee, Jae Wook Oh. Data curation and analysis: Young Geun Kim, Dae Hwan Kim. Writing - original draft: Young Geun Kim. Writing - review & editing: Young Geun Kim, Keun Cheol Lee, Sung Ho Yoon. Approval of the final manuscript: all authors.
Fig. 1.
Intermaxillary fixation (IMF) methods. (A) IMF with arch bars and elastic rubber bands. (B) IMF using screws and elastic bands. The surgeon adjusted the number and position of the IMF screws according to the fracture. Usually, 4-point fixation or 8-point fixation was performed.
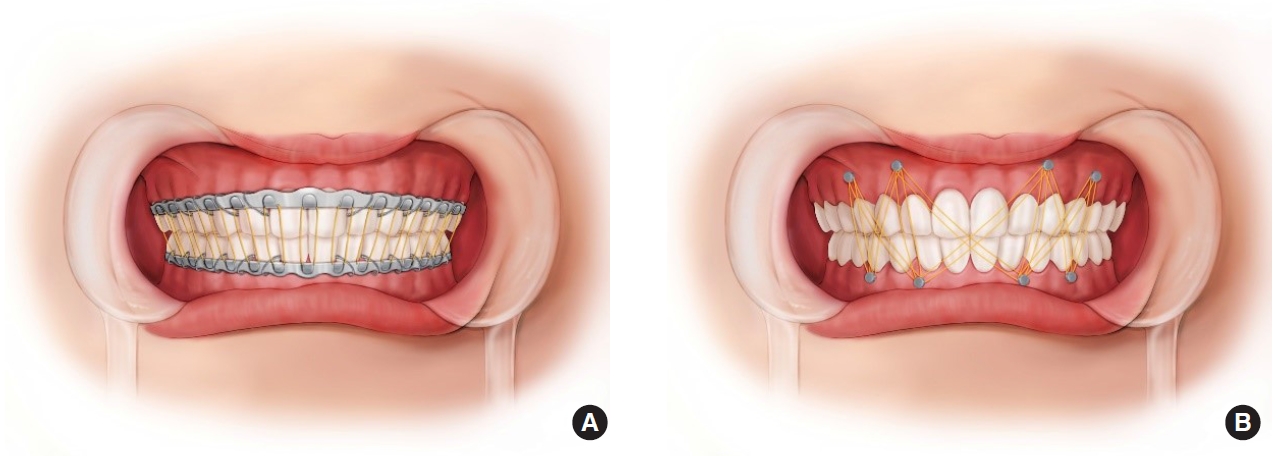
Fig. 2.
A 16-year-old man with mandibular angle fracture. The patient underwent surgery under general anesthesia 2 days after the injury. Intermaxillary fixation (IMF) using screws was performed at 4 points, and then open reduction and internal fixation were performed. IMF was achieved with 4-point fixation using screws and elastic rubber bands. Postoperative intraoral photographs of (A) maxillary side, (B) mandibular side, and (C) frontal views. (D) Postoperative radiography of mandible anteroposterior view.

Fig. 3.
Patient questionnaire and surgeon’s assessment of intermaxillary fixation (IMF). a)Stability of the IMF was assessed as inadequate if there was arch bar loosening or screw loosening; b)Oral hygiene was assessed as inadequate if there was oral debris or calculus.
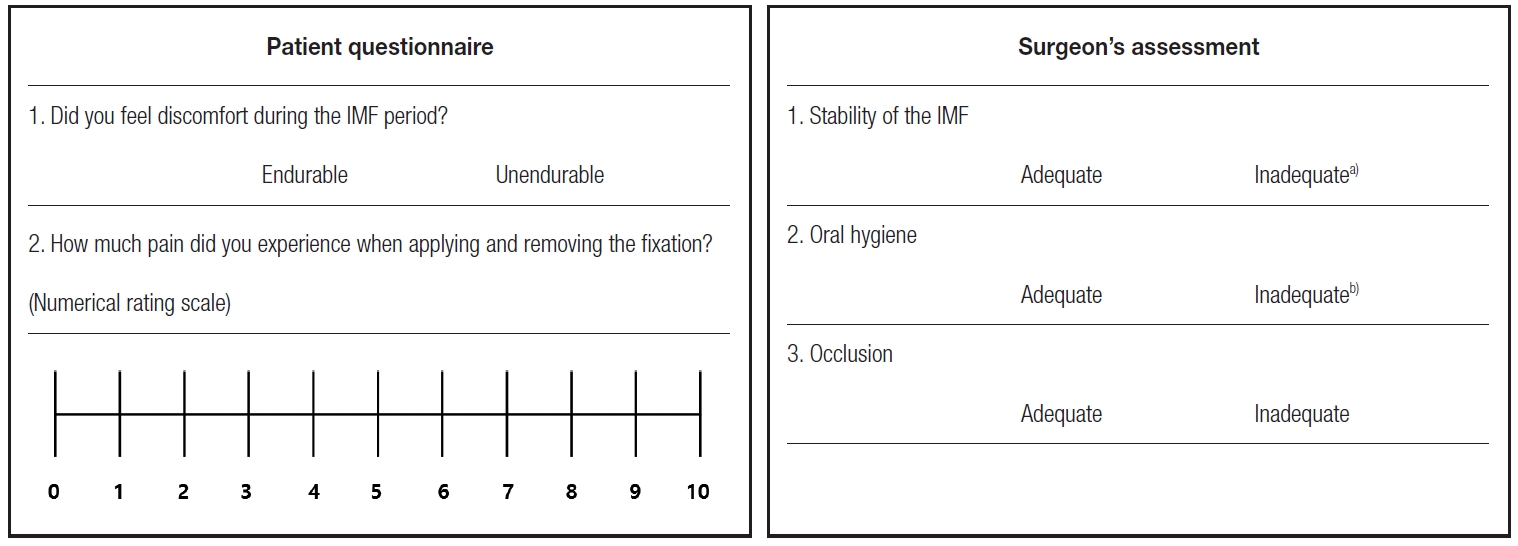
Fig. 4.
Comparison of the intermaxillary fixation (IMF) application time between screws and arch bars. The average time required for IMF was 15.38 minutes in the IMF screw group and 52.41 minutes in the arch bar group (p<0.001).
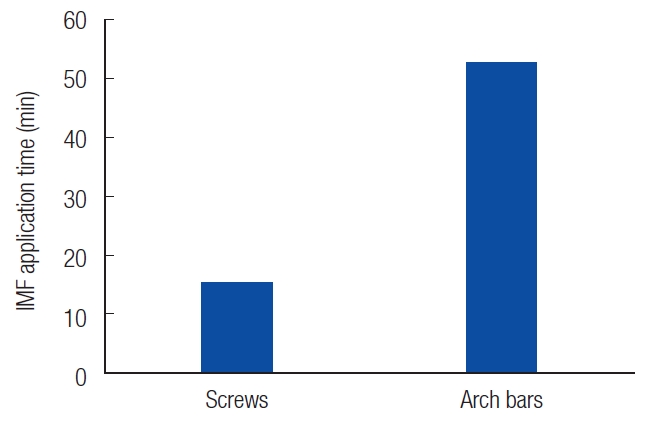
Table 1.
Comparison of intermaxillary fixation (IMF) application time and pain during IMF removal
| Screws (n = 13) | Arch bars (n=31) | p-value | |
|---|---|---|---|
| IMF application time (min) | 15.38 ± 3.20 | 52.41 ± 7.83 | < 0.001a) |
| Pain score during IMF removal | 3.69 ± 0.75 | 5.71 ± 0.82 | < 0.001a) |
Table 2.
Comparison of patient comfort, oral hygiene, intermaxillary fixation (IMF) stability, and occlusion
| Variable | Screws (n = 13) | Arch bars (n = 31) | p-value |
|---|---|---|---|
| Patient discomfort | 0.017a) | ||
| Endurable pain | 11 (84.6) | 14 (45.2) | |
| Unendurable pain | 2 (15.4) | 17 (54.8) | |
| Oral hygiene | 0.015a) | ||
| Adequate | 12 (92.3) | 16 (51.6) | |
| Inadequate | 1 (7.7) | 15 (48.4) | |
| IMF stability | 0.585 | ||
| Adequate | 10 (76.9) | 23 (74.2) | |
| Inadequate | 3 (23.1) | 8 (25.8) | |
| Occlusion | 0.508 | ||
| Adequate | 12 (92.3) | 30 (95.5) | |
| Inadequate | 1 (7.7) | 1 (4.5) |
REFERENCES
1. Stacey DH, Doyle JF, Mount DL, Snyder MC, Gutowski KA. Management of mandible fractures. Plast Reconstr Surg 2006;117:48e-60e.


2. Lee H, Kim KS, Choi JH, Hwang JH, Lee SY. Trauma severity and mandibular fracture patterns in a regional trauma center. Arch Craniofac Surg 2020;21:294-300.



3. Kim YH. Changes and directions of craniofacial surgery in Korea. Arch Craniofac Surg 2019;20:281-3.



5. Choi KY, Yang JD, Chung HY, Cho BC. Current concepts in the mandibular condyle fracture management part I: overview of condylar fracture. Arch Plast Surg 2012;39:291-300.



6. Choi KY, Yang JD, Chung HY, Cho BC. Current concepts in the mandibular condyle fracture management part II: open reduction versus closed reduction. Arch Plast Surg 2012;39:301-8.



- TOOLS
-
METRICS

-
- 4 Crossref
- Scopus
- 5,395 View
- 511 Download
- Related articles in ACFS






