 |
 |
- Search
| Arch Craniofac Surg > Volume 23(2); 2022 > Article |
|
Abstract
Post-traumatic pseudoaneurysms of internal maxillary artery are rare, but may be life-threatening. When arterial damage leads to pseudoaneurysm formation, delayed intractable epistaxis can occur. We report our experience with the diagnosis and management of a ruptured internal maxillary arterial pseudoaneurysm that was discovered preoperatively in a patient with a zygomaticomaxillary complex (ZMC) fracture. He presented to the emergency room with epistaxis, which ceased shortly, and sinus hemorrhage was observed with a fracture of the posterior maxillary wall. The patient was scheduled for open reduction and internal fixation (ORIF) of the ZMC fracture. However, immediately before surgery, uncontrolled epistaxis of unknown origin was observed. Angiography indicated a pseudoaneurysm of the posterior superior alveolar artery. Selective endovascular embolization was performed, and hemostasis was achieved. After radiologic intervention, ORIF was successfully implemented without complications. Our case shows that in patients with a posterior maxillary wall fracture, there is a risk of uncontrolled bleeding in the perioperative period that could be caused by pseudoaneurysms, which should be considered even in the absence of typical symptoms.
Pseudoaneurysm is a rare life-threatening complication; it comprises an arterial wall breach that allows the extravasation of blood into the neighboring tissues [1,2]. A hematoma formed by damage to the arterial wall is replaced by fibrous walls, which expand due to the continuous pulsating pressure and form a pseudoaneurysm [1,3]. Because the wall of a pseudoaneurysm is weaker than that of a true aneurysm, pseudoaneurysms are especially dangerous and have a higher possibility of rupture [4]. Furthermore, the timing of the occurrence of pseudoaneurysms varies after the trauma, which implies that they are likely to go undetected during initial imaging examinations, such as computed tomography (CT) [5].
Only a few cases of preoperatively discovered post-traumatic pseudoaneurysms that affected the internal maxillary artery after a facial bone fracture have been reported. In these cases, the bleeding occurred postoperatively [3,4,6]. Herein, we report a case of intractable epistaxis that occurred just before open reduction and internal fixation (ORIF) in a patient with a zygomaticomaxillary complex (ZMC) fracture.
A 53-year-old man with no significant medical history presented to the emergency department with a comminuted ZMC fracture after an electric kickboard accident. Clinical examination and non-contrast-enhanced CT images revealed sinus hemorrhage with posterior maxillary wall fractures (Fig. 1). There was mild epistaxis, although the bleeding stopped spontaneously after nasal packing. ORIF to repair the ZMC fracture was planned a week later. Common symptoms of pseudoaneurysms such as pulsatile mass, neighboring nerve compression symptoms, typical systolic bruit were not present until the day of the planned surgery; however, on this day, the patient experienced uncontrolled epistaxis of unknown origin. The patientâs vital signs were stable; however, the bleeding did not stop, even with surgical sponge packing. The suspected active bleeding source was a structure posterior to the ZMC. Contrast-enhanced CT images showed damage to the posterior wall of the left maxillary sinus, and contrast agent leaked into the left maxillary sinus. Suspecting rupture of pseudoaneurysm, emergency angiography and endovascular embolization were performed in the interventional radiology department. A ruptured pseudoaneurysm of the posterior superior alveolar artery, originating from the internal maxillary artery, was detected (Fig. 2); accordingly, we performed selective endovascular embolization using Concerto microcoil (Medtronic, Minneapolis, MN, USA) (Fig. 3). Hemostasis was achieved, and the patientâs vital signs were stable. Thirteen days after the endovascular procedure, ORIF was performed successfully under general anesthesia without any complications (Fig. 4). Subciliary, gingivobuccal and lateral eyebrow approach were used and the points of fixation were infraorbital rim, zygomaticomaxillary buttress and frontozygomatic suture. During a follow-up visit 2 months postoperatively, the patient was satisfied with the clinical outcome.
We received written informed consent from the patient for the publication and use of his images, and the study design was approved by the Konyang University Hospital Institutional Review Board (IRB No. 2022-02-005).
Internal maxillary artery is an anatomically complex and difficult structure to handle, with the largest and terminal external carotid arterial branches supplying the deep facial structure. Internal maxillary artery pseudoaneurysms may occur due to complications of trauma or infection associated with maxillofacial surgeries [5]. In previously reported cases, delayed pseudoaneurysms occurred after fracture reduction or orthognathic surgery. However, in the current case, bleeding was observed just before performing an ORIF for a ZMC fracture in a patient who showed no symptoms of a pseudoaneurysm.
A post-traumatic pseudoaneurysm forms when the blood vessel walls are partially ruptured and the blood flow between the arterial laceration and hematoma is maintained. As leakage continues, the hematoma expands; this leads to a pseudoaneurysm [6,7]. Patients may present with delayed epistaxis when arterial damage leads to pseudoaneurysm formation and rupture [8]. Disruption of the maxillary artery and its branches poses a significant threat of continued, delayed epistaxis [5]. In approximately 70% of patients, disruption of the internal maxillary artery or its branches causes uncontrolled epistaxis [9].
Patients with pseudoaneurysm of the internal maxillary artery may exhibit various symptoms, including swelling, facial paralysis, bruit, and an expanding mass [4,9,10]. However, in the current case, there were no symptoms of pseudoaneurysm (other than mild epistaxis) upon arrival to the emergency department. Sudden, uncontrolled epistaxis occurred on the day the ORIF was planned on. The diagnosis of a pseudoaneurysm was made through contrast-enhanced CT and angiography examinations, and selective endovascular embolization was performed as an effective treatment. Had the patient been discharged without exhibiting any symptoms of a pseudoaneurysm, the outcomes would have been fatal in the event of an unexpected massive bleeding.
Facial pseudoaneurysms, in particular, usually form within days to weeks after the occurrence of blunt trauma [6]. The latent period can vary from several days to several years due to a gradual weakening of the arterial wall and erosion of adjacent bones, with most pseudoaneurysms arising within 3 weeks (88%) after the trauma [8]. Thus, predicting the occurrence of pseudoaneurysms may be difficult, because the timing of symptom presentation varies widely. In the current case, it was an event that occurred one week after trauma.
Posterior maxillary walls were known to be difficult to approach because of their anatomical structure [11]. In the current case, the posterior wall of the maxillary sinus was damaged, and a pseudoaneurysm formed in the maxillary sinus. Initially, mild epistaxis (which is considered common in cases of facial fractures) was noted without any other specific findings. Therefore, only reduction surgery for the fracture, without additional diagnosis and treatment for the epistaxis, was planned.
Although post-traumatic pseudoaneurysms of the internal maxillary artery and its branches are rare, they can be life-threatening; thus, their rapid diagnosis and treatment are important [1,3,4,6]. The treatment options for pseudoaneurysms include direct compression, tissue removal, and embolization with selective angiography using contrast agents [6,12]. In the current case, the patient received a radiological intervention for the treatment of the pseudoaneurysm, after which an ORIF was performed to repair the ZMC fracture.
A limitation of our report is that we have described only a single case. Further case reports are required for a complete understanding of the diagnosis and treatment of this condition. Nevertheless, our report provides several lessons regarding the clinical management of such cases. First, it should be noted that uncontrolled massive bleeding can occur at any time, before or after surgery, even if there are no typical symptoms of pseudoaneurysm, in patients with facial fractures. Second, in the case of trauma accompanied by a fracture of the posterior maxillary wall, attention should be paid to pseudoaneurysms caused by vessel injury, which may result in delayed rupture. This can occur before, during, or after facial fracture surgery, and outcomes may be fatal in the absence of a thorough preparation. In conclusion, the risk of uncontrolled bleeding caused by pseudoaneurysms in patients with posterior maxillary wall fractures should be considered in the perioperative period.
Notes
Ethical approval
The study was approved by the Institutional Review Board of Konyang University Hospital (IRB No. 2022-02-005)
Patient consent
The patient provided written informed consent for the publication and the use of his images.
Author contribution
Conceptualization: Soo Yeon Lim. Data curation: Hyun Gun Lee. Formal analysis: Hyun Gun Lee. Project administration: Kyu Nam Kim. Writing - original draft: Hyun Gun Lee. Writing - review & editing: Soo Yeon Lim. Investigation: Hyun Gun Lee. Supervision: Soo Yeon Lim, Hoon Kim, Dong Hyun Oh, In Chang Koh. All authors read and approved the final manuscript.
Fig. 1.
Preoperative computed tomography images show the location of left zygomaticomaxillary complex fracture (red arrow) and hemorrhage area (yellow arrow). (A) Axial image. (B) Sagittal image.
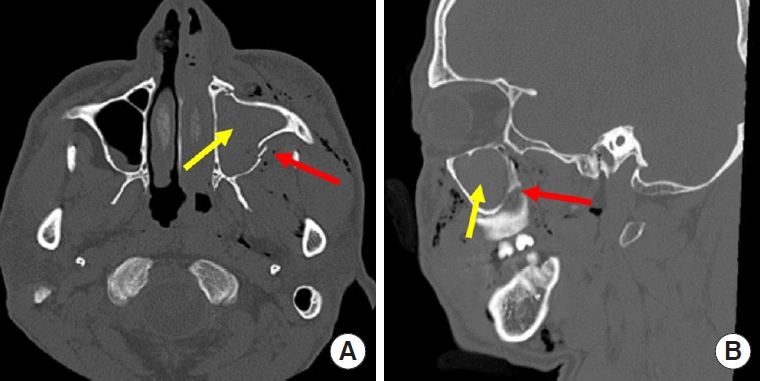
Fig. 2.
Contrast-enhanced computed tomography images show the location of the pseudoaneurysm in the branches of the left internal maxillary artery with sinus hemorrhage (red arrow). (A) Axial image. (B) Sagittal image.
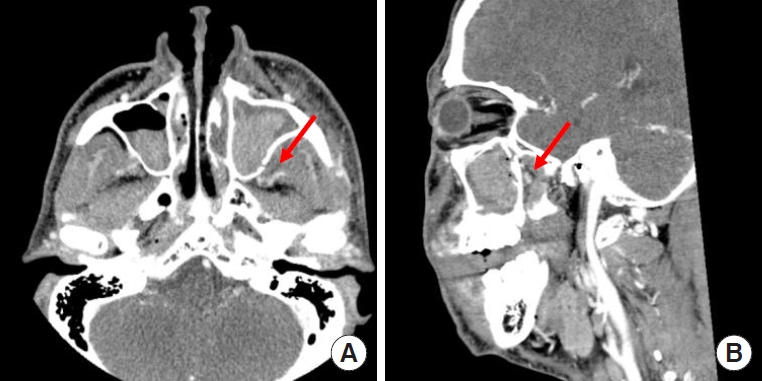
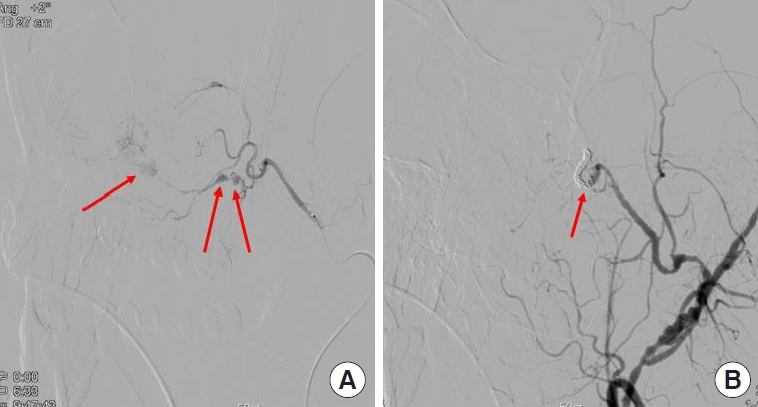
Fig. 3.
Angiographic images. (A) Total of three pseudoaneurysms of the posterior superior alveolar artery (red arrows). A branch of the internal maxillary artery is identified as the bleeding feeder. (B) Through coiling, endovascular embolization of the proximal and distal part of posterior superior alveolar artery was performed, and there was no residual bleeding as soon as the pseudoaneurysms disappeared.
REFERENCES
1. Nastro Siniscalchi E, Catalfamo L, Pitrone A, Papa R, Fama F, Lo Giudice G, et al. Traumatic pseudoaneurysm of the internal maxillary artery: a rare life-threatening hemorrhage as a complication of maxillofacial fractures. Case Rep Med 2016;2016:9168429.



2. Austin RE, Stewart TL, Antonyshyn OM. Intracranial pseudoaneurysm associated with orbitozygomatic complex fracture. J Craniofac Surg 2014;25:1410-2.


3. Chun JJ, Choi CY, Wee SY, Song WJ, Jeong HG. Embolization for treating posttraumatic pseudoaneurysm of the sphenopalatine artery. Arch Craniofac Surg 2019;20:251-4.



4. Alonso N, de Oliveira Bastos E, Massenburg BB. Pseudoaneurysm of the internal maxillary artery: a case report of facial trauma and recurrent bleeding. Int J Surg Case Rep 2016;21:63-6.



5. Luo CB, Teng MM, Chang FC, Chang CY. Role of CT and endovascular embolization in managing pseudoaneurysms of the internal maxillary artery. J Chin Med Assoc 2006;69:310-6.


6. Hwang JH, Kim WH, Choi JH, Kim KS, Lee SY. Delayed rupture of a posttraumatic retromaxillary pseudoaneurysm causing massive bleeding: a case report. Arch Craniofac Surg 2021;22:168-72.



7. Avelar RL, Goelzer JG, Becker OE, de Oliveira RB, Raupp EF, de Magalhaes PS. Embolization of pseudoaneurysm of the internal maxillary artery after orthognathic surgery. J Craniofac Surg 2010;21:1764-8.


8. Willems PW, Farb RI, Agid R. Endovascular treatment of epistaxis. AJNR Am J Neuroradiol 2009;30:1637-45.



9. Fratianne RB, Cocanour CS. Exsanguinating craniofacial trauma. Adv Trauma Crit Care 1992;7:159-73.
10. Al-Saadi NJ, Bakathir A, Al-Mashaikhi A, Al-Hashmi A, Al-Habsi A, Al-Azri F. Maxillary artery pseudoaneurysm as a complication of maxillofacial injuries: report of three cases and literature review. Sultan Qaboos Univ Med J 2019;19:e364-8.



- TOOLS
-
METRICS

-
- 3 Crossref
- Scopus
- 3,557 View
- 107 Download
- Related articles in ACFS







