INTRODUCTION
The bicortical structure among the frontal bones is called the frontal sinus, which is the strongest structure of the skull because it contains two layers of thick bone. Frontal sinus fractures (FSF) are relatively uncommon maxillofacial fractures [
1]. FSF account for 5% to 15% of all maxillofacial traumas, while isolated anterior wall fractures account for one-third of all fractures [
2,
3]. FSF are primarily caused by forces applied directly to the anterior aspect of the skull in the glabellar region. In the anterior wall, the cancellous bone is located between the cortical bones on both sides and thins toward the caudal edge to form the orbital roof. The anterior wall requires a very strong force (800ŌĆō2,200 pounds) for FSF [
4]. However, the posterior wall was relatively thin and directly attached to the dura.
Comminuted fractures of the anterior wall of the frontal sinus are more frequent than simple fractures, as the bone has a significant thickness, and it often causes a contour deformation of the central forehead. However, because the surgical site is in the middle of the forehead, attention must be paid to prevent scarring and nerve injury at the incision site during reduction. The sinus structure is often incompletely reduced, which can lead to a persistent forehead contour deformation. Excessive reduction exacerbates spontaneous fractures. Unless adequate reduction is achieved of FSF, the possibility of intracranial and nasopharyngeal communication through the fracture site persists, which may cause severe infectious complications such as meningitis, brain abscess, and mucocele formation [
5]. A bicoronal incision is classically used to reduce infectious complications of FSF, but it is invasive and has many complications. Therefore, the surgical goal for anterior FSF should be to achieve a satisfactory aesthetic result without scarring or functional complications. A minimally invasive surgical technique for anterior wall reduction of the FSF using a threaded Kirschner wire (T-K wire) or a small incision in the eyebrow has been introduced recently. However, these surgical techniques have some limitations. Therefore, this study aimed to introduce a novel surgical technique for FSF reduction that involves inserting several T-K wires and a periosteal elevator.
METHODS
From January 2012 to December 2021, patients with comminuted and segmental anterior wall FSF who underwent surgery performed by a single surgeon using a T-K wire were recruited. Patients with nasofrontal duct injuries, posterior FSF, open fractures, or other facial fractures were excluded. All patients had apparent forehead depressions but no other hypoesthesia of the supraorbital nerves or external lacerations. After the patientŌĆÖs overall condition was stabilized and soft-tissue swelling of the injured area was reduced, fracture reduction surgery was performed.
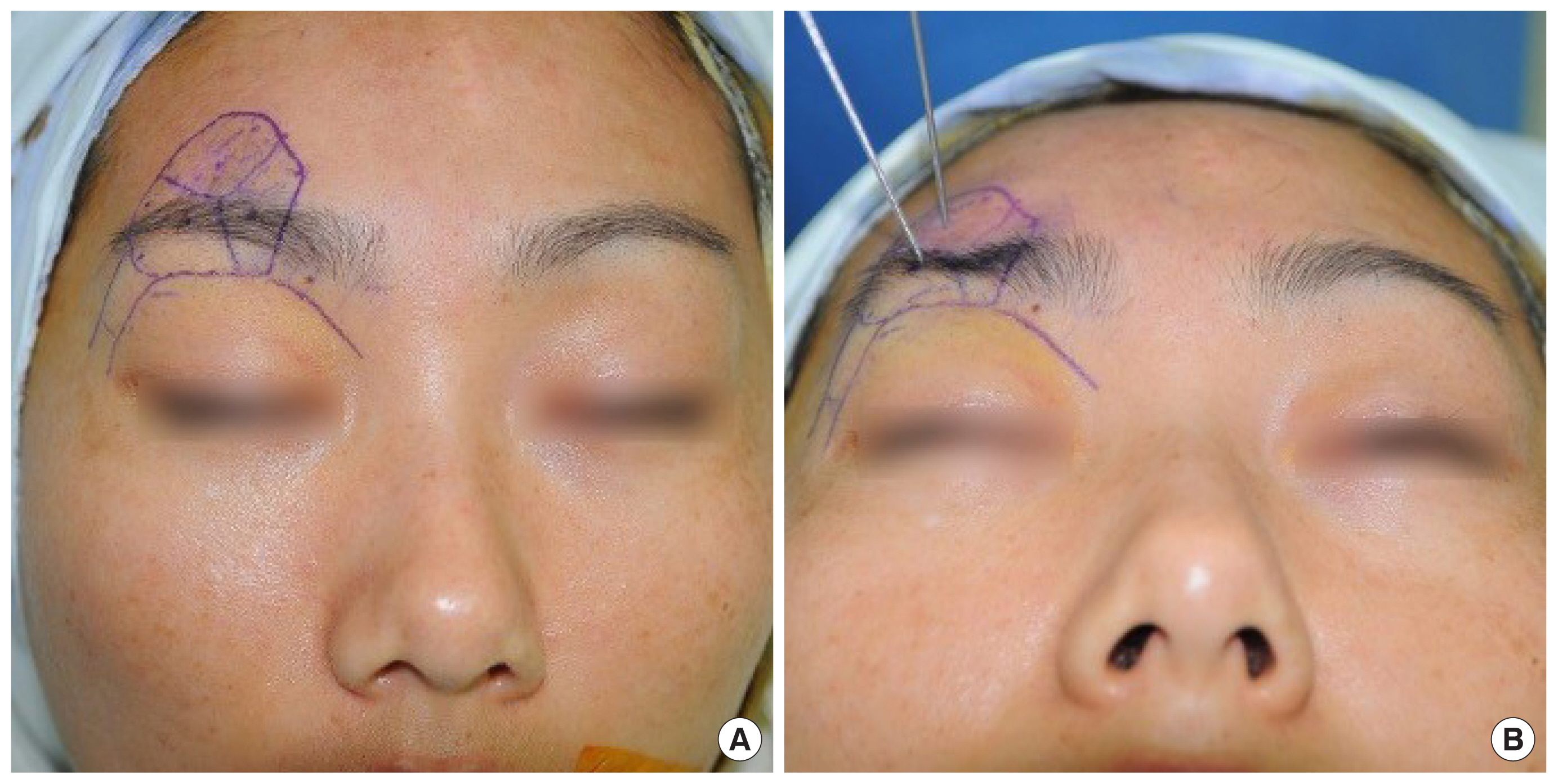
The goal of the surgical technique was to quickly achieve both adequate bone healing and aesthetically pleasing results with ease. Under general anesthesia, each patient was placed in the supine position. The operative field was prepared and draped in the usual manner. The bone segments in the depressed area were marked on three-dimensional computed tomography (3D CT) (
Fig. 1A). The distance from the skin to the posterior wall of the fracture site was measured using the axial view of the 3D CT to avoid brain injury. A fracture line drawing was made mainly around large bone segments to insert a T-K wire, and the distance of each bone segment from the skin to the posterior wall was measured.
After the distance to the T-K wire was indicated using a surgical skin marker, the wire was carefully inserted into each bone segment. When possible, the T-K wire was positioned close to the most severely sunken area to facilitate fracture reduction and placed around a large, more depressed segment (
Fig. 1B). After the skin was penetrated by manual puncturing without drilling, a T-K wire was inserted using a drill once the contour of the anterior wall was touched. The T-K wires were inserted by the selection of well-fixed large bone fragments with the exclusion of unstable bone fragments that were felt by the fingertip or T-K wire tip. To prevent damage to the brain or dura, marked T-K wires were carefully inserted without touching the posterior wall. Subsequently, the fracture fragment was gently pulled with T-K wires that were properly fixed to the bone. Unlike the simple Kirschner wire, the T-K wire had the appropriate pulling force necessary to reduce the FSF.
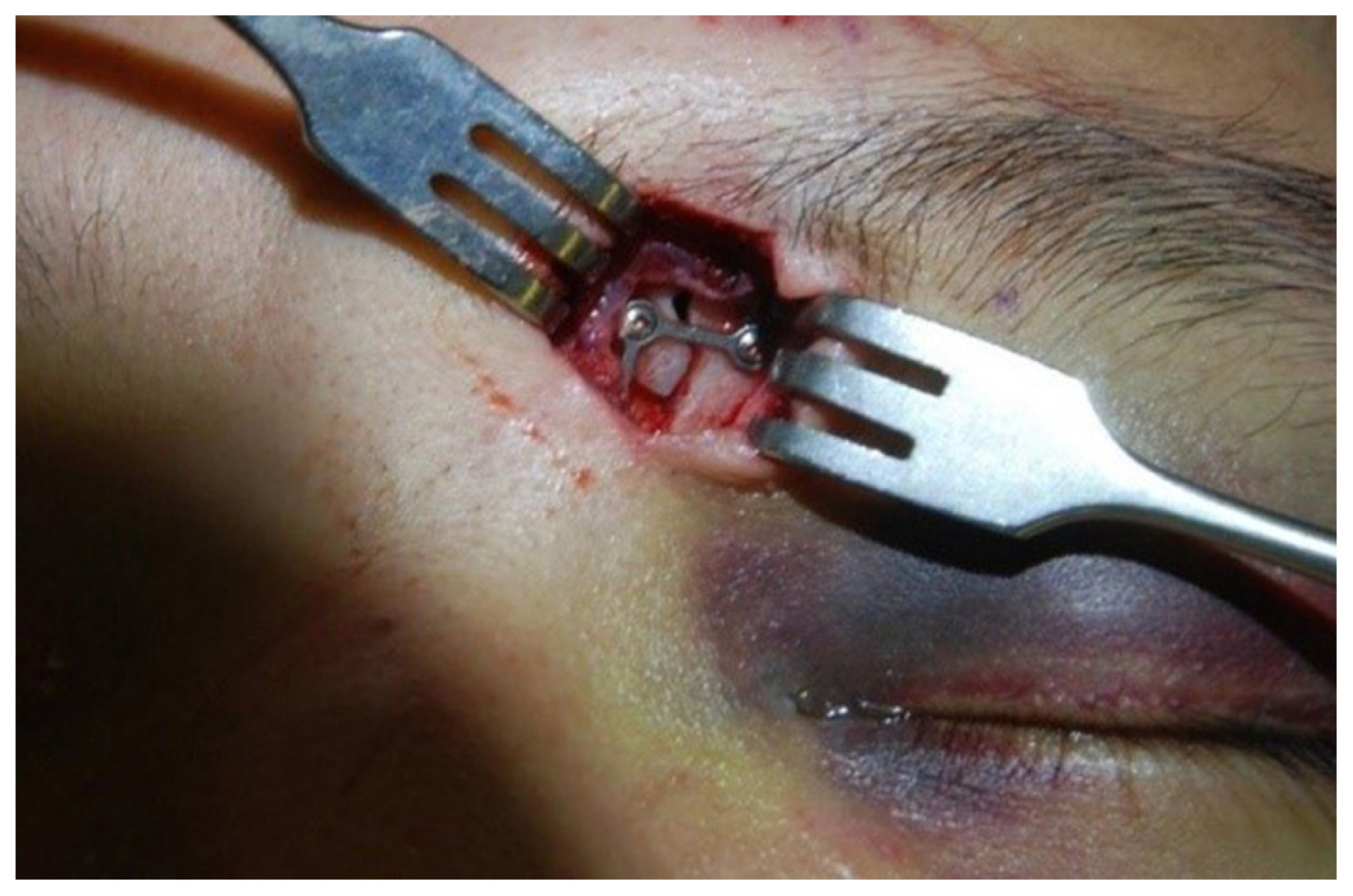
When the reduction force with T-K wires was insufficient, a mini-periosteal elevator was inserted below the fractured anterior wall through a small sub- or supra-brow incision. The reduction was performed using the lever principle by inserting an elevator into the crevasses of the fracture site through a small incision under the eyebrows. If the reduction was unsuccessful, the incision was extended further, the reduction was performed with the elevator with a direct line of sight, and limited fixation was performed with the plate (
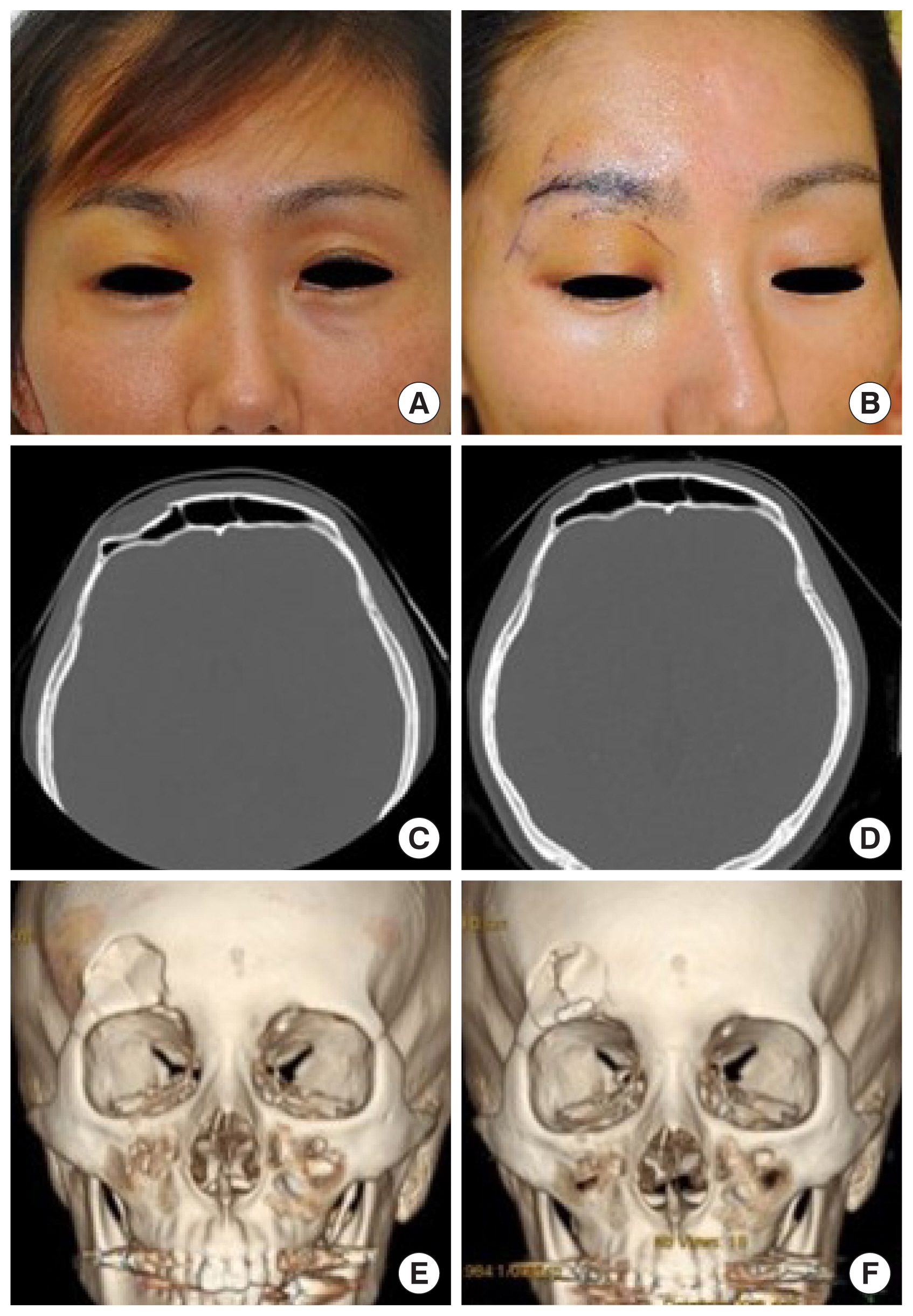
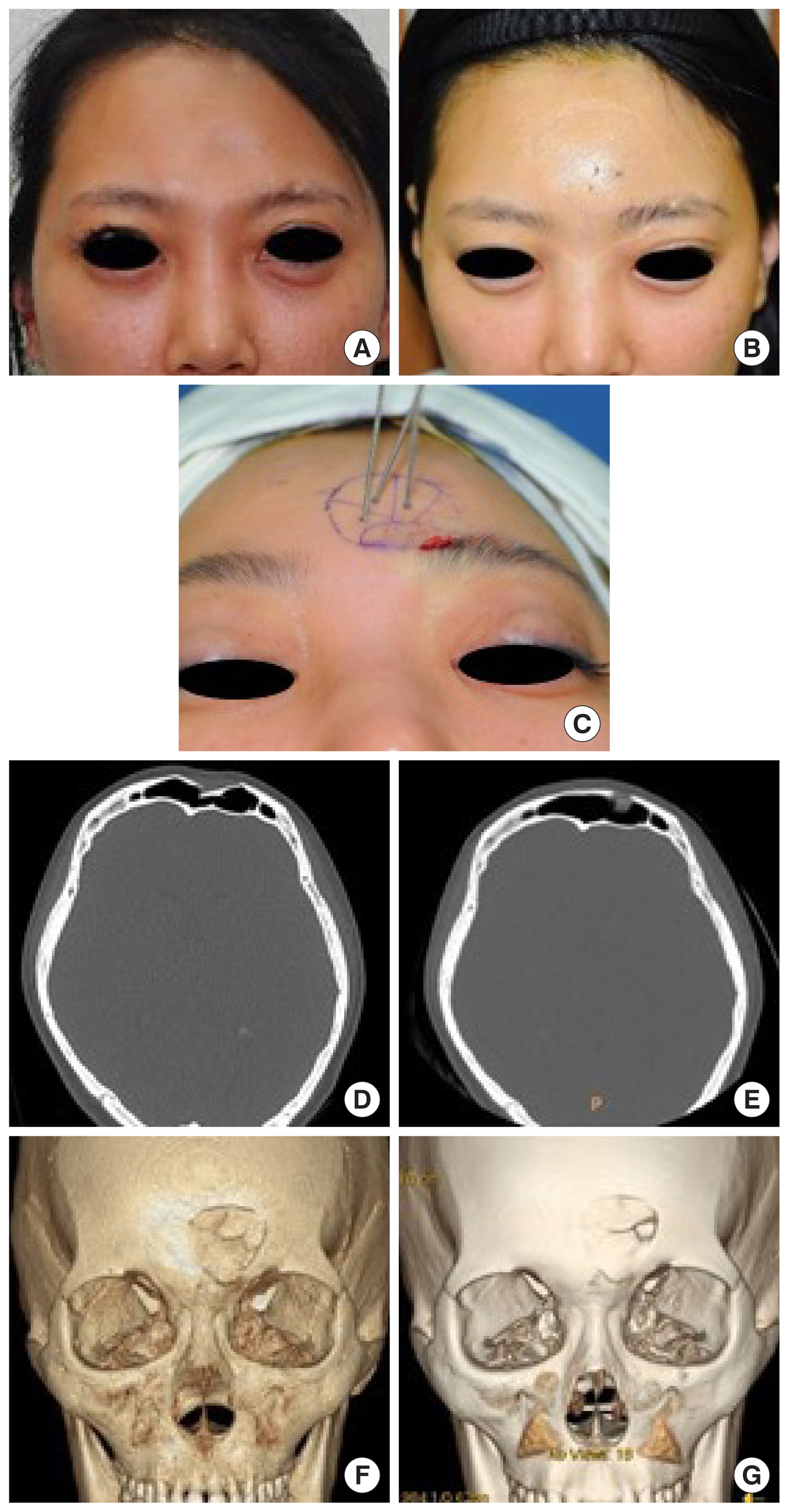
Fig. 2). Once it was confirmed that sufficient reduction had been achieved by palpation with a fingertip, the T-K wires were gently removed. The immediate postoperative results were determined using ultrasonography (
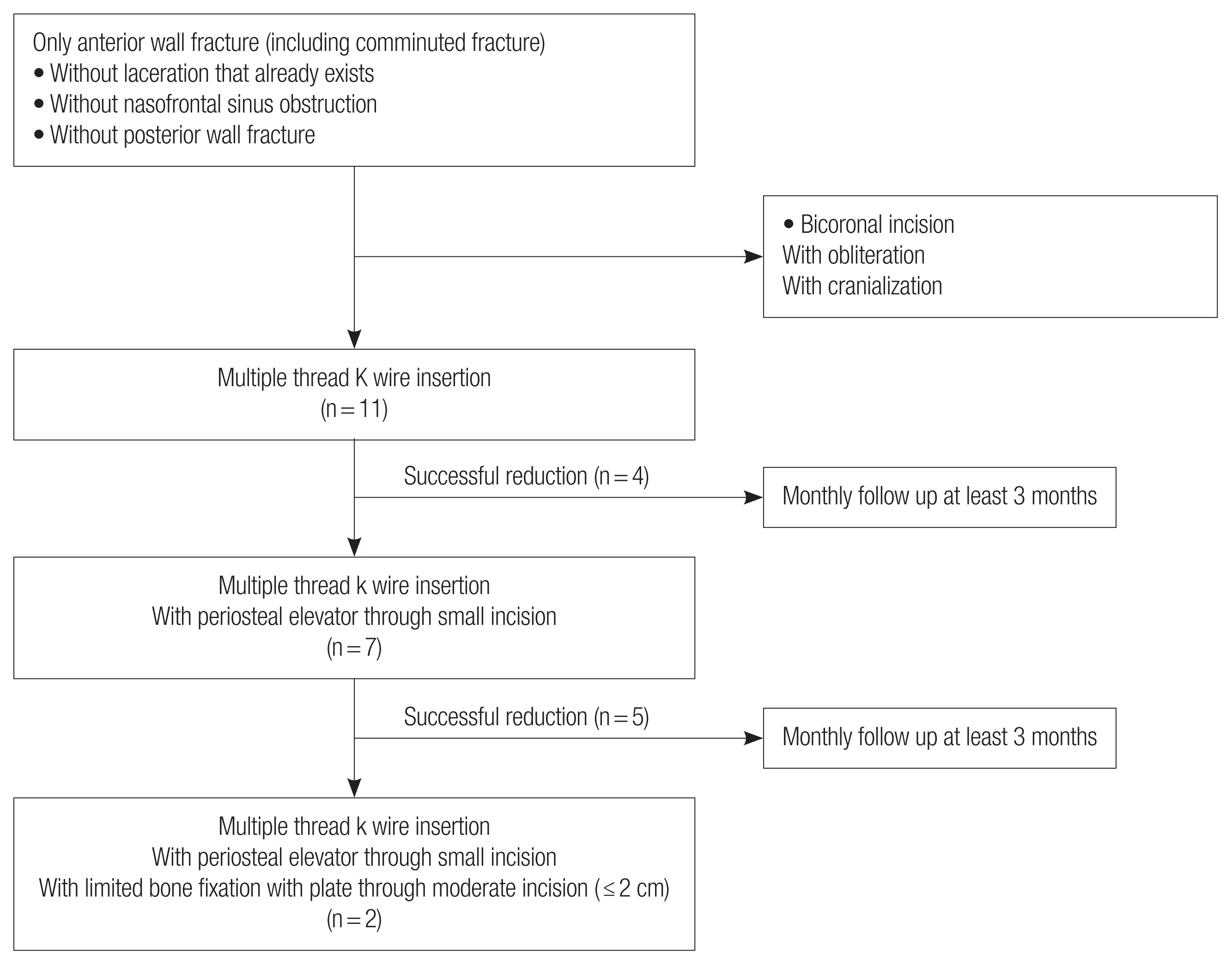
Fig. 3). The algorithm is illustrated in
Fig. 4. Once the reduction results were confirmed, the fracture site was protected for 2 weeks using an Aquaplast (WFR Corp, Ramsey, NJ, USA) splint.
DISCUSSION
After Riedel introduced frontal sinus exenteration in 1898, FSF treatment focused on managing the frontal sinus mucocele. As the surgical technique evolved over time, the reconstruction aimed to achieve an accurate contour of the anterior wall of the FSF, and managing infection has become more important. In 1979, McGrath and Smith [
6] reported anterior FSF surgical success using wires and minimal incisions over a bicoronal incision.
For several decades, the bicoronal incision has been a popular surgical method for FSF. This method is the most common because it involves a large incisional wound. A large dissection range secures a wide field of view, making it ideal for the treatment of extensive fractures. It is also a general approach for FSF obliteration or cranialization [
7,
8]. The coronal approach is associated with complications, such as sensory and motor deficits, scarring on the forehead, and alopecia localized to the scalp [
4].
To avoid these complications, the authors have described various minimally invasive surgical techniques for FSF [
9,
10]. To reduce patient discomfort, increase aesthetic results, and achieve appropriate fracture reduction, less invasive surgery is gradually being performed. These techniques can be divided into two types: external and endoscopic. The external approach is useful if the patient has a laceration at the time of the injury. There is a relatively simple way to access the fracture site by using a periosteal elevator [
11], and it is also possible to access the fracture site by making a small incision in the eyebrow near the fracture site [
12,
13]. An inexperienced surgeon can perform the reduction relatively successfully owing to the ease of access. Although the complications of bicoronal incision can almost be eliminated, facial paresthesia can result. An additional limitation in younger patients is the risk of a noticeable forehead scar.
The endoscope has been widely used since its introduction in 1996 and continues to evolve [
14]. The endoscope allows the approach through the nose and hairline. The hairline approach reduces the fracture site through caudal dissection after an incision is made in the hairline. However, its disadvantages include a long operation time, difficult surgical technique, and incomplete fixation [
15]. In the case of reduction using the transnasal approach, a second sinusotomy is possible [
16]. However, this is true only in cases of non-displaced outer-table fractures, and fixation is difficult. Overall, the endoscopic surgical method has a steep learning curve, and it is difficult to access the upper and lateral sides of the frontal sinus. Moreover, it is difficult to reduce and understand the depth to the posterior wall. In addition, surgery for comminuted fractures is practically impossible. Another disadvantage is that an assistant surgeon must hold the endoscope. Therefore, surgeons face a dilemma in choosing a minimally invasive approach for treating comminuted FSF.
A surgical technique for non-comminuted anterior wall fracture of the frontal sinus using a T-K wire or a small incision in the eyebrow was introduced [
17]. Kim et al. [
18] also introduced a method of percutaneously approaching the frontal anterior wall, inserting a screw, and then treating the fracture through wiring. Bourry et al. [
19] reported reduction and rigid fixation of the anterior wall of the FSF via an upper blepharoplasty incision but that access to the upper and lateral FSF sites was impossible.
However, these methods have disadvantages. When an anterior wall fracture is multiple or segmental, such as in a comminuted fracture, it is difficult to return it to its original shape. Additionally, the fracture fragments could not be elevated despite their strong reduction power, the fracture segments did not return to the normal position, or the fragments were misaligned or dropped into the sinus space. FSF has a thick bone and fractures into multiple segments when subjected to a certain amount of force, limiting surgery to a sub-brow incision or an endoscopic approach. Consequently, successful results were difficult to achieve. Therefore, we attempted to correct the fracture by placing multiple T-K wires on each large fractured bone segment. If the fracture was not elevated by T-K wires, a small periosteal elevator was inserted into the frontal bone cavity through a small incision near the eyebrow and the depressed bone segments were simultaneously elevated. Here we described a simple and effective closed reduction method using multiple T-K wires and small sub-brow incisions.
In many cases of FSF, the bone fragment is dropped owing to tearing of the periosteum or mucosa, resulting in less or more reduction, a common phenomenon in closed reduction. Therefore, it is necessary to simultaneously increase the fracture fragments. However, a significant amount of force is required to simultaneously raise the fracture fragments, and it is difficult to apply the pulling force of the T-K wire, which requires the help of a lever force directly below the fractured fragment. Therefore, in this study, the reduction force was doubled using a periosteal elevator instead of multiple T-K wires. This led to shortened surgical time and effective reduction results. Our surgical technique took approximately 30 minutes, similar to or shorter than that of the other surgical techniques. Also, in terms of confirming the results of surgery, the follow-up 3D CT demonstrated accurate and satisfactory surgical results. Additionally, our procedure is minimally invasive and does not require an assistant surgeon, a disadvantage of endoscopic and bicoronal approach. Therefore, if this surgical method is used efficiently, the bicoronal approach can be avoided in the comminuted FSF, and the operation can be performed more easily and quickly than the endoscopic approach.
Our surgical technique also had certain limitations and risks. First, because the incision is insufficiently applied for rigid fixation, plating to achieve complete fixation is impossible [
20] and the fracture fragment may be more misaligned or fall into the sinus space during surgery. This limitation is common to all FSF surgical methods except bicoronal incision. This can be overcome using a probe method via a real-time navigation guide, which has recently attracted attention [
21,
22]. If the degree of fracture reduction is immediately judged intraoperatively using real-time navigation, an acceptable reduction result can be obtained by increasing the surgical accuracy without rigid fixation. According to a recent literature review, real-time navigation is only sometimes used for surgery using the bicoronal approach for FSF; when the bicoronal approach is combined with this minimally invasive surgical technique, an improved effect is obtained. The second limitation is that the use of a T-K wire can injure the posterior wall, prompting surgeons to carefully avoid serious complications of cerebrospinal fluid leakage. Third, the number of patients in our study (n=11) was insufficient to highlight the surgical methodŌĆÖs merits. A larger multi-institutional study with more patients is needed. Finally, it is necessary to further develop the existing surgical method by combining it with the endoscopic approach developed in this study that is being increasingly used for FSF reduction.
Here we described a simple and effective reduction method using multiple T-K wires and a small sub-brow incision. This surgical method eliminates the disadvantages of bicoronal incision and can compensate for the disadvantages of the endoscopic approach. This surgical technique is efficient for treating comminuted FSF. It is also relatively simple and easy, its results are reliably predicted, and it has the advantage of achieving patient cosmetic satisfaction. A more objective comparison with other surgical methods in more patients is needed in the future.